Defeating Rosacea: 5 Best , Practical & Potent Solutions for Radiant Skin

Overview
Rosacea is a chronic skin condition that primarily affects the face, causing redness, visible blood vessels, and sometimes, small, red bumps resembling acne. It typically occurs in adults and may result in a persistent flushed appearance. Rosacea can vary in severity, with some individuals experiencing mild symptoms while others may develop more pronounced redness and swelling. Although the exact cause of rosacea remains unknown, certain triggers, such as sun exposure, hot beverages, spicy foods, and alcohol consumption, can exacerbate the condition. Treatment options, including topical creams, oral medications, and laser therapy, aim to manage symptoms and improve the overall appearance of the skin.
5 Potent Solutions for Radiant Skin
-
Hydration: Keeping your skin well-hydrated is essential for a radiant complexion. Drink plenty of water throughout the day to maintain skin moisture and suppleness.
-
Skincare Routine: Establish a consistent skincare routine that includes gentle cleansing, exfoliating, and moisturizing. Use products suitable for your skin type to promote a healthy glow.
-
Sun Protection: Shield your skin from harmful UV rays by using sunscreen with a high SPF. Sun protection helps prevent premature aging and reduces the risk of skin damage.
-
Healthy Diet: Consume a balanced diet rich in vitamins, minerals, and antioxidants to nourish your skin from within. Foods like fruits, vegetables, and nuts can contribute to a radiant complexion.
-
Stress Management: Practice stress-relief techniques such as meditation, yoga, or deep breathing to reduce the impact of stress on your skin. Chronic stress can lead to skin issues, so managing it effectively is crucial for radiant skin.
What are the 4 stages of rosacea? :
Rosacea is a chronic skin condition that primarily affects the face, causing redness, visible blood vessels, and acne-like breakouts. It can be a distressing and challenging condition for those who suffer from it, impacting their self-esteem and overall quality of life. Understanding the stages of rosacea is crucial in recognizing and managing the condition effectively.

In this article, we will delve into the four stages of rosacea, providing a comprehensive overview of each stage’s symptoms, causes, and available treatments. By gaining insight into the progression of this condition, individuals can better navigate their own experiences and seek appropriate care. It is important to note that rosacea is a highly individualized condition, and not everyone may progress through all four stages. However, knowing the general progression can help individuals identify potential signs and take proactive measures to maintain skin health and minimize the impact of rosacea on their daily lives.
Through this exploration of the four stages of rosacea, we aim to shed light on the unique challenges faced by individuals with this condition and empower them with knowledge to make informed decisions about their skincare and treatment options. By understanding the underlying causes and triggers, individuals can work with healthcare professionals to develop personalized approaches that manage symptoms and enhance their overall well-being.
Stage 1: Pre-rosacea
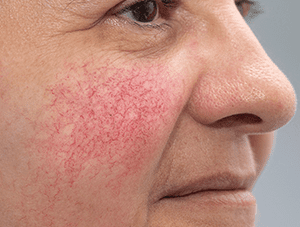
At this initial stage, individuals may experience occasional facial flushing and persistent redness. The skin might feel sensitive and show signs of increased reactivity to various triggers such as sunlight, heat, or certain foods. Small blood vessels on the face, known as telangiectasia, may become more visible. However, there are usually no other noticeable symptoms of rosacea at this stage.
Stage 2: Mild Rosacea
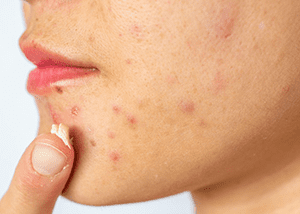
During this stage, the redness of the face becomes more pronounced and persistent. Flushing episodes may occur frequently, and small red bumps known as papules might develop. Some individuals may also experience stinging or burning sensations on their skin. This stage of rosacea can often be mistaken for acne or other skin conditions.
Stage 3: Moderate Rosacea

In the moderate stage of rosacea, the symptoms become more prominent and widespread. Persistent redness intensifies, and the skin may develop pustules, which are small, pus-filled bumps. Swelling and inflammation may also occur, leading to a thicker and coarser appearance of the skin. Ocular rosacea, which affects the eyes, can also manifest at this stage, causing dryness, redness, and a gritty sensation.
Stage 4: Severe Rosacea
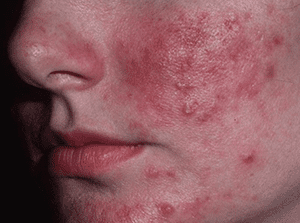
Severe rosacea is the most advanced stage of the condition. The symptoms are highly visible and can significantly impact a person’s appearance and self-confidence. In addition to persistent redness, severe flushing, and prominent bumps, the skin may develop nodules and cysts. The nose may also become enlarged and bulbous, a condition known as rhinophyma. Ocular rosacea symptoms can worsen, leading to further discomfort and potential vision problems.
How do you know if you have rosacea? :

Diagnosing rosacea requires a medical evaluation by a dermatologist or healthcare professional. However, there are some common signs and symptoms that can indicate the presence of rosacea. Persistent facial redness, especially on the central areas of the face, is a hallmark sign. This redness may resemble a blush or sunburn that does not fade away. Other signs include the presence of visible blood vessels (telangiectasia) on the face, the development of small red bumps or pustules, and a persistent feeling of warmth or burning on the skin. If you experience any of these symptoms, it is important to consult a healthcare professional for an accurate diagnosis and appropriate treatment options.
Recognizing the symptoms of rosacea and seeking early medical intervention can help individuals manage the condition effectively and prevent its progression to more advanced stages. It is important to remember that rosacea is a chronic condition, but with proper care and treatment, individuals can minimize the impact of symptoms on their daily lives and maintain healthy, balanced skin.
Rosacea Symptoms

Rosacea is characterized by a variety of symptoms that can vary in severity from person to person. The most common symptom is facial redness, which often appears as a persistent flush or blush on the cheeks, nose, forehead, and chin. This redness is caused by the dilation of blood vessels close to the skin’s surface. In addition to redness, individuals with rosacea may experience other symptoms such as visible blood vessels (telangiectasia), a sensation of heat or burning on the skin, and swelling or inflammation. Some individuals may also develop small red bumps and pustules that resemble acne.
Rosacea Skin Conditions

Rosacea can lead to several skin conditions as the condition progresses. One common skin condition associated with rosacea is known as rosacea-induced acne. This type of acne is characterized by small, red, and inflamed bumps that may contain pus. These bumps can be similar in appearance to traditional acne but are typically not accompanied by blackheads or whiteheads. Another skin condition associated with rosacea is thickening of the skin, known as dermal fibrosis. In some cases, the skin may become rough, bumpy, and develop a thicker texture.
Rosacea Flare-ups
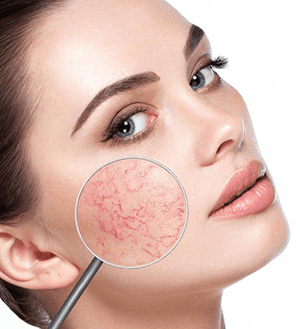
Rosacea flare-ups are episodes in which the symptoms of the condition become more pronounced and intense. These flare-ups can be triggered by various factors, including exposure to sunlight, extreme temperatures (hot or cold), wind, certain foods and beverages (such as spicy foods, alcohol, or caffeine), emotional stress, and certain skincare products. During a flare-up, individuals may experience a sudden increase in redness, a burning or stinging sensation, and the appearance of new bumps or pustules. Flare-ups can be unpredictable and may vary in duration and intensity from person to person.
What are the main causes of rosacea? :
The main causes of rosacea are multifactorial and include genetic predisposition, abnormalities in facial blood vessels, an overactive immune system, and the presence of certain microorganisms on the skin. While the exact mechanisms and interactions between these factors are not fully understood, they contribute to the development and progression of rosacea.

Genetic factors play a significant role in rosacea, as it tends to run in families. Abnormalities in facial blood vessels, such as dilation and increased permeability, contribute to the redness and inflammation associated with rosacea. An overactive immune system triggers an inflammatory response, leading to the characteristic symptoms of rosacea. In addition, certain microorganisms, particularly Demodex mites that naturally reside on the skin, may contribute to the development of rosacea by triggering immune responses.
It’s important to note that these factors can vary in their influence from person to person. While some individuals may have a strong genetic predisposition to rosacea, others may be more affected by immune system dysregulation or microorganism-related triggers. Understanding these underlying causes can help individuals manage their condition more effectively by avoiding triggers, seeking appropriate treatment, and making lifestyle adjustments that promote overall skin health.
Rosacea Causes

The exact cause of rosacea is still unknown, but several factors are believed to contribute to its development. One significant factor is genetic predisposition. Studies have shown that rosacea tends to run in families, suggesting a genetic component to the condition. Abnormalities in the blood vessels are also thought to play a role. Facial blood vessels may dilate and become more permeable in individuals with rosacea, leading to redness and inflammation.
Additionally, an overactive immune system and chronic inflammation are believed to be involved in the development of rosacea. The immune system’s response to various triggers may cause inflammation in the skin, contributing to the characteristic symptoms of rosacea. Lastly, certain microorganisms, such as Demodex mites that naturally reside on the skin, have been associated with rosacea. These mites may trigger immune responses and further contribute to the development and progression of the condition.
Rosacea Triggers

Identifying triggers is crucial for managing rosacea and preventing flare-ups. While triggers can vary among individuals, some common ones have been identified. Exposure to sunlight is a common trigger for many people with rosacea. UV rays can cause blood vessels to dilate, leading to increased redness and inflammation. Extreme temperatures, both hot and cold, can also trigger flare-ups.
Wind, especially when combined with cold temperatures, can further irritate the skin. Certain foods and beverages have been reported to worsen rosacea symptoms. Spicy foods, alcohol, and hot beverages are known triggers for many individuals. Additionally, emotional stress and intense physical exercise can lead to flushing and increased blood flow to the skin, aggravating rosacea symptoms.
Rosacea and Diet

While the impact of diet on rosacea is still being studied, certain dietary factors have been identified as potential triggers for some individuals. Spicy foods, such as chili peppers and hot sauces, have been reported to exacerbate rosacea symptoms in some people. Similarly, hot beverages, such as coffee and tea, can contribute to flushing and increased redness in the face.
Alcohol is another common trigger for rosacea flare-ups. Red wine, in particular, has been linked to worsening symptoms. Additionally, certain histamine-rich foods, such as aged cheese, fermented products, and cured meats, have been reported to trigger rosacea in some individuals who are sensitive to histamine.
While these triggers may affect some individuals with rosacea, it’s important to note that triggers can vary from person to person. Keeping a diary to track personal triggers can be helpful in identifying and avoiding specific foods and beverages that worsen rosacea symptoms. Working with a healthcare professional or a registered dietitian can also provide guidance on dietary modifications that may help manage the condition.
Is rosacea hard to diagnose? :
Diagnosing this condition can pose challenges due to its resemblance to other skin conditions and variations in its presentation. The symptoms can overlap with acne, seborrheic dermatitis, and other skin disorders. Additionally, the signs and symptoms can fluctuate, making it more challenging to diagnose during periods of remission.
The absence of specific diagnostic tests further complicates the process. However, with the expertise of dermatologists and a thorough evaluation of clinical signs, medical history, and physical examination, an accurate diagnosis can be made.
It is essential for individuals experiencing symptoms suggestive of this condition to seek medical attention from a qualified healthcare professional for an appropriate diagnosis and personalized treatment plan.
Rosacea Diagnosis
Diagnosing this skin condition can be challenging due to its resemblance to other skin conditions. Dermatologists rely on clinical observations, medical history, and physical examination to make an accurate diagnosis. They look for signs like persistent facial redness, visible blood vessels, and acne-like bumps. Additional symptoms such as flushing, stinging, and eye irritation are also assessed. A comprehensive evaluation helps differentiate this condition from others and ensure an accurate diagnosis.
Rosacea vs Acne
While this condition and acne may appear similar, they are distinct conditions. Acne is characterized by comedones (whiteheads and blackheads) and typically affects oilier areas like the forehead, nose, and chin. On the other hand, this condition primarily affects the central part of the face, featuring persistent redness, flushing, and visible blood vessels. Unlike acne, this condition doesn’t involve comedone formation. Distinguishing between the two is crucial as they require different treatment approaches.
Rosacea Misdiagnosis
Misdiagnosis of this condition is common due to its resemblance to other skin conditions. One frequent misdiagnosis is acne or acne vulgaris, especially in cases of papulopustular rosacea. This misdiagnosis can result in ineffective treatment and delays in addressing the underlying condition.
Another misdiagnosis is seborrheic dermatitis, which shares similarities with this condition, including facial redness and scaling. However, seborrheic dermatitis primarily affects areas with higher sebum production, such as the scalp, eyebrows, and nasolabial folds.
It’s crucial for healthcare professionals to be aware of these potential misdiagnoses and carefully consider symptoms and clinical presentation to arrive at an accurate diagnosis.
Can rosacea be prevented? :
Taking preventive measures can significantly reduce the risk of developing this chronic skin condition. Individuals with a family history of the condition or those prone to facial redness should be proactive in their approach to minimize the chances of developing it.
Avoiding triggers such as excessive sun exposure, extreme temperatures, spicy foods, and alcohol can help prevent flare-ups and reduce the likelihood of developing the condition.
Maintaining a consistent and gentle skincare routine, along with proper sun protection measures, is crucial in managing and potentially preventing the onset of the condition.
While there is no guaranteed way to completely prevent the condition, following these preventive measures and working closely with healthcare professionals can help individuals minimize the impact and manage the symptoms effectively.
Preventing the Condition
Taking preventive measures can help minimize the risk of developing this chronic skin condition. Individuals with a family history of the condition or those prone to facial redness should be proactive in their approach.
Avoiding triggers such as sun exposure, extreme temperatures, spicy foods, and alcohol can significantly reduce the likelihood of flare-ups. Maintaining a consistent skincare routine with gentle products suited for sensitive skin is crucial.
Additionally, managing stress levels and incorporating relaxation techniques can contribute to overall skin health and potentially prevent the onset of the condition.
Sun Protection for the Skin
Using sun protection measures is essential in managing this dermatological condition. Individuals should prioritize using broad-spectrum sunscreens with high SPF to shield their skin from harmful UV rays.
Look for physical blockers like zinc oxide or titanium dioxide, as they are less likely to irritate the skin. Applying sunscreen generously and regularly, especially before sun exposure, is essential in protecting the skin.
Additionally, utilizing protective clothing, such as wide-brimmed hats and sunglasses, can provide additional defense against the sun’s rays. Incorporating these sun protection measures into daily routines can help minimize the impact of sun-induced flare-ups.
Skincare Routine for Managing the Condition
Establishing a proper skincare routine is crucial for individuals with this skin condition. Gentle cleansing is key, using mild, fragrance-free products to avoid further irritation.
Harsh scrubbing or exfoliation should be avoided as they can exacerbate symptoms. Opt for non-comedogenic and hypoallergenic moisturizers to keep the skin hydrated without clogging the pores.
It is important to avoid skincare products containing potential irritants such as alcohol, fragrance, or harsh chemicals. Working with a dermatologist can help determine the most suitable skincare routine, including specific products and ingredients that cater to individual needs.
What treatment is good for rosacea? :
When it comes to finding effective treatments for this condition, it’s important to consider individual factors such as the severity of symptoms, medical history, and personal preferences. The treatment plan may involve a combination of approaches tailored to address the specific needs of each individual.
Medical treatments, including topical medications, oral antibiotics, and prescription creams, are commonly prescribed to manage symptoms such as inflammation and redness. These treatments work to address the underlying causes of the condition and provide relief.
Laser therapy is another effective treatment option for reducing visible blood vessels and redness. By using targeted beams of light, laser treatment can selectively destroy abnormal blood vessels while minimizing damage to the surrounding skin.
In addition to medical interventions, lifestyle modifications and self-care practices play a crucial role in managing the condition. This can include dietary adjustments, such as avoiding trigger foods, and adopting a gentle skincare routine using suitable products for sensitive skin.
It’s important to note that the effectiveness of treatments can vary among individuals. What works well for one person may not yield the same results for another. Therefore, consulting with a healthcare professional, such as a dermatologist, is vital to receive a proper diagnosis and develop a tailored treatment plan that suits the individual’s specific condition.
Remember, managing this condition is a journey, and finding the right treatment approach may require some trial and error. With the guidance of healthcare professionals and a comprehensive treatment plan, individuals can effectively manage their symptoms and improve their quality of life.
Treating the Condition
Managing this chronic skin condition involves a variety of treatment options. The choice of treatment depends on the severity of the symptoms and the individual’s specific needs.
Medical interventions, such as topical medications, oral antibiotics, or prescription creams, are commonly prescribed to control inflammation and reduce redness. These medications work by targeting the underlying causes of the condition and providing relief from symptoms.
In addition to medical treatments, various natural remedies can complement the treatment plan. Natural remedies like green tea extracts, chamomile, and aloe vera have anti-inflammatory properties and can soothe the skin. However, it is important to consult with a healthcare professional before incorporating any natural remedies to ensure their safety and efficacy.
Laser Treatment for the Condition
Laser therapy is a popular and effective treatment option for managing this dermatological condition. Laser treatment involves using a focused beam of light to target and reduce visible blood vessels, redness, and skin thickening. The laser energy selectively destroys the abnormal blood vessels while minimizing damage to the surrounding skin.
Laser treatment sessions are typically spaced out over a period of several weeks to achieve optimal results. The procedure may cause temporary discomfort, redness, or swelling, but these side effects generally subside quickly.
It is important to note that laser treatment may not be suitable for everyone, and its effectiveness can vary depending on individual factors. Consulting with a dermatologist or skincare professional is crucial to determine if laser treatment is a viable option and to ensure the best course of treatment for each individual.
Diet and Lifestyle for Managing the Condition
Diet and lifestyle modifications can play a role in managing this skin condition. While there is no specific “rosacea diet,” certain foods and beverages may trigger flare-ups in some individuals. Common triggers include spicy foods, alcohol, hot beverages, and foods high in histamines.
Maintaining a well-balanced diet that includes plenty of fruits, vegetables, lean proteins, and whole grains can help support overall skin health. Staying hydrated and practicing stress management techniques, such as meditation or yoga, can also contribute to reducing symptoms.
Furthermore, individuals should avoid excessive sun exposure, extreme temperatures, and harsh skincare products that may irritate the skin. Using gentle cleansers, moisturizers, and sunscreen with a high SPF is recommended as part of a skincare routine.
Medications for Managing the Condition
In more severe cases, healthcare professionals may prescribe oral medications to help control the symptoms and reduce inflammation. Antibiotics, such as tetracycline or doxycycline, may be prescribed to manage the inflammatory response and control bacterial growth. Other oral medications, such as isotretinoin, may be used in certain cases to regulate oil production and reduce inflammation.
It’s important to follow the prescribed dosage and duration of medication as instructed by the healthcare professional. Regular follow-up appointments are typically scheduled to monitor the effectiveness of the medication and make any necessary adjustments.
Natural Remedies for Symptom Relief
In addition to medical treatments, some individuals may find relief from natural remedies that can help soothe the skin and reduce inflammation. These can include herbal extracts, such as chamomile or green tea, which have anti-inflammatory properties. Applying cool compresses or using gentle, fragrance-free skincare products can also help alleviate symptoms.
However, it’s important to note that natural remedies may not work for everyone, and their effectiveness can vary. It’s advisable to consult with a healthcare professional before incorporating any natural remedies into the treatment plan to ensure they are safe and suitable for the individual.
Laser Treatment for Visible Blood Vessels
For individuals with visible blood vessels and persistent redness, laser treatment can be an effective option. Laser therapy uses targeted beams of light to selectively heat and destroy abnormal blood vessels, thereby reducing redness and improving overall skin appearance.
The laser treatment sessions are typically spaced out over several weeks, allowing the skin to heal between sessions. While the procedure may cause some temporary redness or discomfort, these side effects are usually mild and subside quickly.
Laser treatment can provide long-lasting results, but it may require multiple sessions depending on the severity of the condition. It’s important to consult with a dermatologist or skincare professional to determine if laser treatment is appropriate for the individual and to discuss the potential benefits and risks.
Dietary Considerations
While there is no specific “rosacea diet,” some dietary choices may help manage the condition. Certain foods and beverages, such as spicy foods, alcohol, hot beverages, and histamine-rich foods, can trigger flare-ups in some individuals. It may be beneficial to keep a food diary to identify any potential triggers and make dietary adjustments accordingly.
Maintaining a well-balanced diet rich in fruits, vegetables, lean proteins, and whole grains can support overall skin health. Staying hydrated and incorporating stress-reducing techniques, such as meditation or yoga, may also help minimize symptoms.
It’s important to note that dietary changes alone may not be sufficient to manage the condition, and they should be complemented with other treatment approaches. Consulting with a healthcare professional or registered dietitian can provide personalized guidance on dietary considerations and their potential impact on the individual’s condition.
Home Remedies and Self-Care Practices
In addition to medical treatments and lifestyle modifications, self-care practices can contribute to managing the condition. This can include gentle skincare routines using mild cleansers, moisturizers, and sunscreen suitable for sensitive skin. Avoiding harsh chemicals, fragrances, and abrasive scrubbing can help prevent further irritation.
Applying cool compresses to the affected areas or taking lukewarm baths can provide relief during flare-ups. Avoiding excessive sun exposure, extreme temperatures, and known triggers can also help minimize symptoms.
It’s important to keep in mind that self-care practices alone may not be sufficient to manage the condition, especially in more severe cases. It’s advisable to work in collaboration with a healthcare professional to develop a comprehensive treatment plan that incorporates both medical interventions and self-care practices.
Remember, each individual’s condition is unique, and what works for one person may not work for another. Consulting with a healthcare professional or dermatologist is crucial to receive a proper diagnosis and develop a personalized treatment plan that addresses the specific needs and goals of the individual.
Related Links
Conclusion
In conclusion, the condition discussed in this article is a chronic dermatological condition that primarily affects the face. While it can be a challenging condition to manage, there are various treatment options available to alleviate symptoms and improve the overall quality of life for individuals affected by it.
The condition’s causes are not yet fully understood, but factors such as genetics, environmental triggers, and an overactive immune system are believed to play a role. Recognizing the symptoms, which can include facial redness, visible blood vessels, acne-like breakouts, and eye irritation, is crucial for an accurate diagnosis.
Diagnosing the condition can sometimes be challenging, as its symptoms can overlap with other skin conditions such as acne. Seeking medical advice from a dermatologist or healthcare professional is essential to receive an accurate diagnosis and develop a personalized treatment plan.
Treatment options vary and may include medications, laser therapy, lifestyle modifications, and self-care practices. The choice of treatment depends on the severity of symptoms and individual needs. It’s important to consult with healthcare professionals to determine the most suitable approach and make informed decisions.Â
Q: 1. What are the main causes of this condition?
A : The exact causes are not fully understood, but factors such as genetic predisposition, environmental triggers, and immune system abnormalities are believed to contribute to the development of the condition.
Q: 2. Can this condition be cured completely?
A : While there is no known cure, effective management strategies are available to control symptoms and minimize flare-ups. With proper treatment and lifestyle adjustments, many individuals can experience significant improvement in their symptoms.
Q: 3. Are there any natural remedies for managing the condition?
A : Some individuals may find relief from natural remedies such as chamomile, green tea, and aloe vera, which have anti-inflammatory properties. However, it’s important to consult with a healthcare professional before incorporating any natural remedies into the treatment plan.
Q: 4. What role does diet play in managing the condition?
A : While there is no specific “condition diet,” certain foods and beverages may trigger flare-ups in some individuals. It may be helpful to keep a food diary to identify potential triggers and make dietary adjustments accordingly.
Q: 5. Is laser treatment effective for reducing redness and visible blood vessels?
A : Yes, laser treatment can be an effective option for reducing redness and visible blood vessels associated with the condition. Laser therapy targets and destroys abnormal blood vessels while minimizing damage to the surrounding skin.
More Links


