Eczema Relief: 5 Best , Practical & Powerful Solutions to Calm the Itch

Overview
Eczema is a chronic skin condition that causes red, inflamed, and itchy patches to appear on the skin. It is a common condition that can affect people of all ages, but it is most often seen in infants and young children. Eczema can be triggered or worsened by various factors, including dry skin, irritants, allergens, stress, and weather changes. While there is no cure for eczema, there are various treatments and self-care measures available to manage the symptoms and reduce flare-ups, providing relief and improving the quality of life for those affected by this skin condition.
5 Potent Solutions to Calm the Itch :
-
Moisturize Regularly: Keeping the skin well-hydrated is essential to alleviate eczema-related itching. Apply a thick, hypoallergenic moisturizer or emollient multiple times a day to lock in moisture and soothe the skin.
-
Avoid Triggers: Identify and avoid potential triggers that may worsen eczema symptoms and lead to itching. These triggers can include certain fabrics, soaps, detergents, and allergens. Opt for gentle, fragrance-free products to reduce irritation.
-
Use Topical Steroids: For more severe cases of itching, dermatologists may recommend the short-term use of topical corticosteroids. These creams or ointments can effectively reduce inflammation and itching, but they should be used under medical supervision.
-
Take Warm Baths: Soaking in a lukewarm bath with added colloidal oatmeal or baking soda can help calm itchy skin. Avoid hot water, as it can strip the skin of its natural oils and exacerbate eczema symptoms.
-
Cold Compresses: Applying a cold, damp cloth or a cool compress to affected areas can provide immediate relief from itching. Cold compresses can help reduce inflammation and soothe the skin.
Remember that individual responses to eczema treatments may vary, so it’s essential to work closely with a healthcare provider or dermatologist to determine the best course of action for managing eczema and its associated itching.
Introduction
Eczema is a common skin condition that affects people of all ages. Its symptoms can vary in intensity and presentation, often causing discomfort and frustration for those who experience them. In this article, we will delve into the various symptoms associated with eczema, including itchy rash, dry skin, red patches, and flaky scalp. Additionally, we will explore the five key symptoms of eczema in detail.
Eczema, also known as atopic dermatitis, is a chronic inflammatory skin condition characterized by dry, itchy, and inflamed patches of skin. It is not contagious and is believed to be influenced by a combination of genetic and environmental factors. While eczema can occur at any age, it commonly appears in early childhood and may persist into adulthood.
What Are The 5 Symptoms of Eczema? :

-
Intense Itching: Eczema is accompanied by severe itching, which can disrupt daily activities and sleep patterns. Scratching the affected areas can cause further damage and increase the risk of infection.
-
Redness and Inflammation: The skin affected by eczema often appears red, inflamed, and swollen. These visible signs are a result of increased blood flow and inflammation in the affected areas.
-
Dry and Irritated Skin: Eczema leads to dry, rough, and scaly skin. The compromised skin barrier makes it difficult for the skin to retain moisture, resulting in dryness and irritation.
-
Blisters or Crusting: In some cases, eczema can cause the development of small, fluid-filled blisters that may ooze and crust over. These blisters can be particularly uncomfortable and may lead to further skin damage if scratched.
-
Thickened and Leather-Like Skin: With prolonged and untreated eczema, the skin can become thickened and take on a leathery texture. This symptom, known as lichenification, occurs due to constant scratching and rubbing of the affected areas.
Itchy Rash

One of the hallmark symptoms of eczema is an intensely itchy rash. The affected areas of skin may appear red, inflamed, and swollen. The constant urge to scratch can lead to further irritation and even skin damage. Scratching the rash can worsen symptoms and potentially introduce infections.
An intensely itchy rash is a hallmark symptom of eczema, a chronic skin condition that affects millions of people worldwide. When someone with eczema experiences an outbreak, their skin becomes red, inflamed, and swollen, causing considerable discomfort. The itchiness associated with the rash can be overwhelming and persistent, leading to an intense urge to scratch.
The constant scratching can worsen the symptoms and create a vicious cycle. Initially, scratching may provide temporary relief, but it ultimately exacerbates the condition. The repeated mechanical friction on the skin can further irritate the already inflamed areas, causing them to become even more red, swollen, and tender. Additionally, scratching can lead to micro-tears in the skin, compromising its integrity and making it more susceptible to infection.
Dry Skin

Dryness is another prevalent symptom of eczema. The skin affected by eczema tends to lose moisture easily, leading to a compromised skin barrier. As a result, the skin becomes more susceptible to irritants and allergens, exacerbating the condition.
Dry skin is a common and bothersome symptom experienced by individuals with eczema. The skin affected by eczema tends to have a decreased ability to retain moisture, leading to a dry and dehydrated appearance. This dryness occurs due to the impaired functioning of the skin barrier, which plays a crucial role in maintaining skin hydration.
In individuals with eczema, the skin barrier becomes compromised, allowing moisture to escape more easily. This compromised barrier function is often a result of genetic factors and abnormalities in proteins that are essential for maintaining skin integrity. As a result, the skin loses moisture and becomes dry, rough, and scaly.
Red Patches

Eczema often presents as red, inflamed patches on the skin. These patches can vary in size and location, depending on the individual and the severity of the condition. The redness is caused by increased blood flow and inflammation in the affected areas.
Red patches are a common and noticeable symptom of skin conditions like eczema. When a person experiences an eczema flare-up, their skin becomes inflamed, leading to the appearance of distinct red patches. These patches can vary in size and location, depending on the individual and the severity of the condition.
The redness observed in eczema patches is primarily a result of increased blood flow and inflammation in the affected areas. Inflammation is the body’s natural response to injury or irritation, and in the case of eczema, it is triggered by an overactive immune system. The immune system mistakenly identifies certain substances or triggers as threats, leading to an inflammatory response.
Flaky Scalp
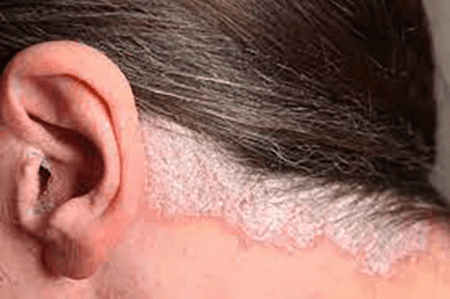
In addition to affecting the body, eczema can also manifest on the scalp. Flaky scalp is a common symptom, characterized by dry, scaly patches or dandruff-like flakes. The itchiness can be particularly bothersome, leading to discomfort and self-consciousness.
When eczema affects the scalp, it can lead to a flaky scalp, which is a common and troublesome symptom. Flaky scalp in eczema presents as dry, scaly patches or dandruff-like flakes on the scalp. This condition, known as scalp eczema or seborrheic dermatitis, can cause discomfort and self-consciousness.
The flakes on the scalp are a result of the skin’s increased turnover rate and the accumulation of dead skin cells. In eczema, the skin’s natural shedding process becomes disrupted, leading to a buildup of dry, flaky skin on the scalp. These flakes can range in size from small, fine particles to larger, more noticeable scales. The scalp may also appear red, inflamed, and irritated, contributing to the overall discomfort.
What is the main cause of eczema? :
The exact cause of eczema is not fully understood, but it is believed to be a complex interplay of genetic, environmental, and immune system factors. Eczema is considered a multifactorial condition, meaning it is influenced by a combination of genetic predisposition and external triggers.
People with a family history of eczema are more likely to develop the condition, suggesting a genetic component. Certain genes have been identified as being associated with eczema susceptibility. These genes can affect the skin’s barrier function, immune response, and inflammatory pathways, making individuals more prone to developing eczema.

Environmental factors also play a significant role in the development of eczema. Exposure to certain allergens, irritants, or microbes can trigger or worsen eczema symptoms. Common environmental triggers include allergens like pollen, pet dander, and dust mites, as well as irritants such as harsh soaps, detergents, and chemicals. Additionally, changes in temperature, humidity, and exposure to certain fabrics or clothing materials can also contribute to eczema flare-ups.
The immune system dysfunction is another important factor in eczema. In individuals with eczema, the immune system reacts abnormally to certain substances, leading to inflammation and the characteristic symptoms of eczema. This immune dysregulation can result in an overactive immune response, causing chronic inflammation in the skin.
While the main cause of eczema is multifaceted, understanding the genetic, environmental, and immune system factors involved can help guide treatment strategies and management approaches for individuals with eczema. A comprehensive approach that addresses these factors, such as avoiding triggers, managing stress, and maintaining a healthy lifestyle, can help reduce the frequency and severity of eczema flare-ups and improve overall skin health.
Allergies
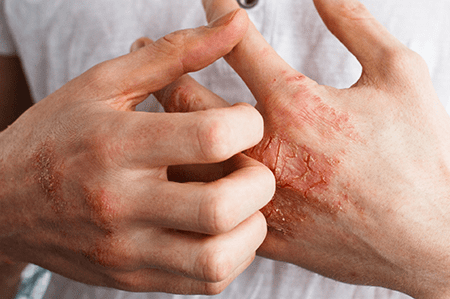
Allergies play a significant role in the development and exacerbation of eczema. Many individuals with eczema have allergic sensitivities to various substances, known as allergens. Common allergens that can trigger eczema flare-ups include certain foods (such as dairy products, eggs, nuts, and wheat), pollen, dust mites, pet dander, and certain fabrics.
When someone with eczema comes into contact with an allergen, their immune system overreacts, leading to an inflammatory response in the skin. This immune response can cause itching, redness, and the formation of eczema patches. Identifying and avoiding allergens that trigger eczema can help individuals manage their symptoms effectively.
In some cases, healthcare professionals may recommend allergy testing to determine specific allergens to avoid. This testing can involve skin prick tests or blood tests to identify the specific substances that trigger an allergic reaction in the individual. Once identified, allergens can be avoided through dietary modifications, changes in the living environment, and lifestyle adjustments. Additionally, healthcare professionals may recommend medications or immunotherapy (allergy shots) to help desensitize the immune system and reduce the severity of allergic reactions.
Genetics

Genetics plays a crucial role in the development of eczema. It is widely acknowledged that eczema tends to run in families, and individuals with a family history of eczema have a higher risk of developing the condition. Researchers have identified specific genes that are associated with eczema susceptibility.
Variations in these genes can affect the skin’s barrier function, immune response, and inflammatory pathways, making individuals more susceptible to eczema. However, it’s important to note that genetics alone do not determine whether someone will develop eczema. Other factors, such as environmental triggers and immune system dysfunction, also contribute to the development of the condition.
Understanding the genetic factors involved in eczema can help researchers develop targeted treatments and interventions in the future. For individuals with a family history of eczema, it may be beneficial to be proactive in managing their skin health and taking preventive measures to minimize exposure to known triggers. While genetic factors play a role, it is also important to address environmental and lifestyle factors to effectively manage and reduce eczema symptoms.
Stress
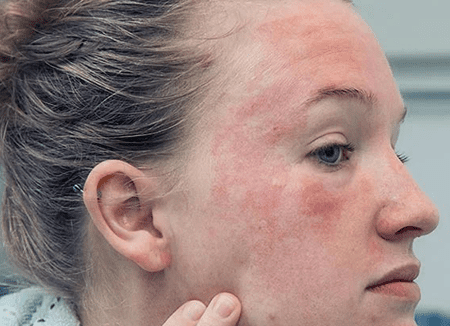
Stress is a significant factor that can trigger or exacerbate eczema symptoms. When someone experiences stress, their body releases stress hormones, such as cortisol, which can disrupt the immune system and contribute to inflammation. For individuals with eczema, stress can act as a trigger, leading to flare-ups or worsening of existing symptoms.
Furthermore, the itchiness and discomfort associated with eczema can cause emotional stress, creating a cyclical relationship between stress and eczema symptoms. Managing stress through relaxation techniques, mindfulness practices, exercise, and seeking support from healthcare professionals or support groups can help individuals with eczema reduce the impact of stress on their condition.
In addition to stress management, it is important for individuals with eczema to maintain a healthy lifestyle that includes a balanced diet, regular exercise, and sufficient sleep. Taking care of overall well-being can help strengthen the immune system and improve the skin’s ability to cope with triggers and reduce the frequency and severity of eczema flare-ups.
What is the first diagnosis of eczema? :
The first diagnosis of atopic dermatitis, commonly known as eczema, often occurs in childhood. It is a chronic condition characterized by periods of flare-ups and remission. Typically, the diagnosis is made based on the appearance and distribution of the skin lesions, along with a history of persistent itching and recurrent skin symptoms.
In infants and young children, atopic dermatitis commonly affects the face, scalp, and extensor surfaces of the limbs. The affected areas may exhibit redness, dryness, and scaling. The skin may appear rough and thickened due to scratching and rubbing. Intense itching is a hallmark symptom of eczema.
The diagnosis is primarily clinical, based on the characteristic appearance and distribution of the skin lesions. However, a detailed medical history is also crucial in the diagnosis process. The healthcare professional will inquire about the child’s symptoms, their duration, and any known triggers or factors that worsen the symptoms. They may also inquire about the family history of atopic dermatitis or other allergic conditions, as there is a genetic predisposition for the condition.
The first diagnosis of eczema can be challenging for both patients and parents. However, early recognition and diagnosis are essential for appropriate management and treatment. Healthcare professionals play a crucial role in providing support, education, and guidance to help individuals and their families manage the condition effectively and improve the quality of life for those with atopic dermatitis.
Eczema Diagnosis
Eczema, also known as atopic dermatitis, is diagnosed through a combination of medical history, physical examination, and, in some cases, additional tests. The diagnosis is made by a healthcare professional, typically a dermatologist or allergist, who specializes in skin conditions.
During the medical history assessment, the healthcare professional will ask about the patient’s symptoms, their duration and frequency, any known triggers or aggravating factors, and the family history of eczema or other allergic conditions. This information helps establish the likelihood of atopic dermatitis as the cause of the symptoms.
A thorough physical examination is conducted to assess the skin’s appearance and characteristics. The healthcare professional will examine the affected areas of the skin, looking for specific signs and symptoms of atopic dermatitis, such as redness, dryness, scaling, thickening, and the presence of lesions or blisters. They will also assess other areas of the body to identify any additional areas of involvement.
In some cases, additional tests may be recommended to confirm the diagnosis or rule out other possible causes of the symptoms. These tests can include skin patch tests, blood tests to measure specific antibodies or immune system markers, and skin biopsies to examine a small sample of the affected skin under a microscope.
What is the best protection for eczema? :
The best protection for atopic dermatitis lies in a combination of strategies that help manage the condition and minimize flare-ups. Here are some key aspects to focus on for effective eczema protection:
-
Skincare Routine: Establish a consistent skincare routine that includes gentle cleansing, moisturization, and avoidance of triggers. This helps maintain the skin’s barrier function, prevent dryness, and minimize inflammation.
-
Moisturize Regularly: Moisturize the skin daily using fragrance-free and hypoallergenic moisturizers. Apply moisturizer immediately after bathing to lock in moisture. Regular moisturization helps keep the skin hydrated and reduces itching and irritation.
-
Avoid Triggers: Identify and avoid triggers that worsen eczema symptoms. These can include irritants like certain fabrics, harsh soaps, or chemicals. Allergens such as dust mites, pet dander, or pollen can also trigger flare-ups. Minimizing exposure to these triggers can help protect the skin.
-
Clothing Choices: Opt for soft, breathable fabrics like cotton and avoid tight-fitting clothing that can cause friction and irritation. Choose clothing without harsh dyes or chemicals that can irritate the skin.
-
Environmental Control: Maintain a clean and allergen-free environment. Regularly clean bedding, vacuum carpets, and use air purifiers to reduce dust and allergens. Maintain appropriate humidity levels in the home to prevent excessive dryness or humidity that can trigger eczema.
By implementing these protective measures, individuals with atopic dermatitis can effectively manage their condition and minimize the frequency and severity of flare-ups. It is important to work closely with a healthcare professional to develop a personalized management plan that suits individual needs and preferences.
Skincare Routine
A proper skincare routine is essential for individuals with atopic dermatitis, also known as eczema. The goal of a skincare routine is to maintain the skin’s hydration, strengthen the skin barrier, and minimize triggers that can exacerbate eczema symptoms. Here are some key components to consider when establishing a skincare routine:
-
Gentle Cleansing: Use mild, fragrance-free cleansers that are specifically formulated for sensitive skin. Avoid harsh soaps or cleansers that can strip the skin of its natural oils and further dry out the skin.
-
Moisturization: Moisturizers play a crucial role in managing eczema. Choose fragrance-free, hypoallergenic moisturizers that contain ingredients like ceramides, hyaluronic acid, or shea butter. Apply moisturizer immediately after bathing and throughout the day as needed to keep the skin hydrated and prevent dryness.
-
Avoiding Triggers: Identify and avoid triggers that worsen eczema symptoms. These can include certain fabrics, irritating chemicals, harsh detergents, or allergens. Opt for soft, breathable fabrics like cotton and avoid tight-fitting clothing that can cause friction and irritation.
-
Bathing Practices: Take lukewarm baths or showers for short durations to avoid excessive drying of the skin. Pat the skin dry gently with a soft towel instead of rubbing. Immediately apply moisturizer to seal in the moisture.
-
Sun Protection: Protect the skin from the sun’s harmful UV rays by using broad-spectrum sunscreen with a high SPF. Choose sunscreens that are specifically formulated for sensitive skin and are free of fragrances or harsh chemicals.
Clothing Choices
The choice of clothing can greatly impact individuals with atopic dermatitis. Wearing the right clothing can help reduce irritation, promote comfort, and minimize the risk of triggering eczema flare-ups. Here are some tips for choosing clothing for eczema-prone skin:
-
Opt for Soft Fabrics: Choose soft, natural fabrics like cotton and silk. These fabrics are gentle on the skin, breathable, and less likely to cause irritation compared to synthetic materials.
-
Loose-Fitting Clothing: Wear loose-fitting clothing that allows the skin to breathe. Tight clothing can cause friction and irritation, exacerbating eczema symptoms. Avoid clothing with tight elastic bands or rough seams.
-
Avoid Harsh Dyes and Chemicals: Look for clothing that is free of harsh dyes, chemicals, and fragrances. These additives can irritate sensitive skin and trigger eczema flare-ups. Wash new clothing before wearing to remove any residual chemicals.
-
Layering: Layer clothing to adjust to changes in temperature and humidity. This allows you to add or remove layers as needed without overheating or exposing the skin to extreme weather conditions.
-
Protect Hands and Feet: Wear gloves or mittens during cold weather to protect the hands, and choose breathable socks and shoes that allow for air circulation to prevent excessive sweating and moisture buildup.
Moisturizers
Moisturizers are a vital component of managing atopic dermatitis. They help hydrate the skin, restore the skin barrier, and reduce itching and dryness. Here are some considerations when selecting and using moisturizers for eczema-prone skin:
-
Choose the Right Type: Look for moisturizers specifically formulated for sensitive or eczema-prone skin. These moisturizers are often fragrance-free, hypoallergenic, and gentle on the skin. Options include creams, ointments, or lotions.
-
Ingredients to Look For: Opt for moisturizers that contain ingredients such as ceramides, hyaluronic acid, shea butter, or glycerin. These ingredients help replenish moisture, strengthen the skin barrier, and soothe dry and irritated skin.
-
Regular Application: Apply moisturizer immediately after bathing while the skin is still damp. This helps lock in moisture and prevents excessive drying. Reapply moisturizer throughout the day, especially after washing hands or when the skin feels dry.
-
Patch Test: If trying a new moisturizer, perform a patch test on a small area of the skin before applying it all over. This helps ensure that the moisturizer does not cause any adverse reactions or irritate the skin further.
-
Individual Preferences: Every individual may have different preferences when it comes to moisturizers. Experiment with different brands and formulations to find the one that works best for your skin. Some individuals may prefer thicker ointments for intense hydration, while others may prefer lighter lotions for daily use.
What is the best medicine for eczema? :
When it comes to the best medicine for atopic dermatitis, there is no one-size-fits-all answer. Treatment options vary depending on the severity of the condition, individual response, and the recommendations of a healthcare professional. Here are some common medications prescribed for atopic dermatitis:
-
Topical Corticosteroids: These medications are commonly prescribed to reduce inflammation and relieve itching. They come in varying strengths and forms, such as creams, ointments, or lotions. Topical corticosteroids are typically applied directly to the affected areas and used for short durations as directed by a healthcare professional.
-
Topical Calcineurin Inhibitors: These medications, such as tacrolimus and pimecrolimus, are alternatives to corticosteroids. They work by suppressing the immune response and reducing inflammation. Topical calcineurin inhibitors are often prescribed for sensitive areas or when corticosteroids are not suitable.
-
Systemic Medications: In severe cases or when topical treatments are not sufficient, oral medications or injections may be prescribed. These systemic medications, such as oral corticosteroids or immunosuppressants, work to reduce inflammation throughout the body.
-
Biologic Therapies: Biologic drugs, such as dupilumab, are newer treatment options for moderate to severe atopic dermatitis. These medications target specific molecules involved in the immune response and inflammation.
The choice of medicine depends on several factors, including the individual’s age, medical history, severity of symptoms, and response to previous treatments. It is important to work closely with a healthcare professional or dermatologist to determine the most appropriate medicine and develop a comprehensive treatment plan for atopic dermatitis.
Eczema Cream
Eczema creams play a vital role in managing the symptoms of atopic dermatitis. These topical treatments help soothe and moisturize the skin, reduce inflammation, and alleviate itching. There are various types of eczema creams available, and the choice depends on the severity of the condition and individual preferences. Here are some common types of eczema creams:
-
Moisturizers: Moisturizing creams or ointments are an essential part of eczema management. These products help replenish the skin’s moisture and strengthen the skin barrier. Look for fragrance-free, hypoallergenic moisturizers that contain ingredients like ceramides, hyaluronic acid, or shea butter.
-
Topical Corticosteroids: These creams contain corticosteroids, which help reduce inflammation and itching. They are available in various strengths, and their usage should be guided by a healthcare professional. It is important to use topical corticosteroids as prescribed and follow the instructions carefully to avoid potential side effects.
-
Topical Calcineurin Inhibitors: These creams inhibit the activity of immune cells involved in inflammation. They are often used as an alternative to corticosteroids, especially in sensitive areas like the face or groin. Topical calcineurin inhibitors are effective in reducing inflammation and controlling eczema symptoms.
-
Barrier Repair Creams: These creams contain ingredients that help repair and strengthen the skin barrier. They are particularly beneficial for individuals with compromised skin barrier function. Barrier repair creams typically contain ceramides, fatty acids, or other lipid-based ingredients.
The choice of eczema cream depends on the individual’s specific needs and the severity of their atopic dermatitis. It is important to consult with a healthcare professional or dermatologist to determine the most suitable cream and develop a personalized treatment plan.
Natural Remedies
Many individuals with atopic dermatitis seek natural remedies as complementary approaches to manage their condition. While natural remedies may provide relief for some people, it is essential to remember that they may not work for everyone and should be used under the guidance of a healthcare professional. Here are some natural remedies that are commonly explored for eczema:
-
Coconut Oil: Coconut oil is a natural moisturizer that can help hydrate the skin and reduce dryness and itching. It contains fatty acids that have anti-inflammatory properties. Apply virgin coconut oil directly to the affected areas to soothe the skin.
-
Oatmeal Baths: Adding colloidal oatmeal to lukewarm baths can provide relief from itching and inflammation. Colloidal oatmeal helps to soothe and moisturize the skin. Soak in the oatmeal bath for around 15-20 minutes and gently pat the skin dry afterward.
-
Honey: Honey has antimicrobial and anti-inflammatory properties that can help alleviate eczema symptoms. It can be applied topically to the affected areas or added to bathwater for soothing relief. However, individuals with a known allergy to honey should avoid using it.
-
Evening Primrose Oil: Evening primrose oil is derived from the seeds of the evening primrose plant and contains gamma-linolenic acid (GLA). GLA is an omega-6 fatty acid that has anti-inflammatory properties. It is available in supplement form and may help reduce eczema symptoms.
While natural remedies may provide relief for some individuals, it is important to note that scientific evidence supporting their effectiveness is limited. It is recommended to consult with a healthcare professional before trying any natural remedies to ensure their safety and appropriateness for individual circumstances.
Eczema Diet
Diet can play a role in managing atopic dermatitis, and some individuals may find that certain foods trigger or worsen their eczema symptoms. However, it is important to note that food triggers can vary from person to person, and not all individuals with atopic dermatitis will have dietary sensitivities. Here are some considerations when it comes to an eczema diet:
-
Identifying Triggers: Keep a food diary to identify potential triggers. Common culprits include dairy products, eggs, nuts, soy, wheat, and certain fruits or vegetables. Eliminate suspected trigger foods from your diet for a few weeks and reintroduce them one at a time to observe any changes in symptoms.
-
Anti-inflammatory Foods: Include foods that have anti-inflammatory properties in your diet. These can include fatty fish rich in omega-3 fatty acids (such as salmon or sardines), leafy greens, turmeric, ginger, and foods high in antioxidants like berries.
-
Hydration: Drink plenty of water to stay hydrated and maintain overall skin health. Proper hydration can help prevent dryness and reduce the risk of eczema flare-ups.
-
Balanced Diet: Focus on a balanced diet that includes a variety of fruits, vegetables, whole grains, lean proteins, and healthy fats. A well-rounded diet provides essential nutrients that support overall skin health.
It is important to remember that dietary changes should be made in consultation with a healthcare professional or a registered dietitian. They can provide guidance and help determine if any specific dietary modifications are necessary based on individual needs and potential triggers.
How can I get rid of eczema fast at home? :
Getting rid of atopic dermatitis entirely at home can be challenging, as it is a chronic condition that requires long-term management. However, there are several strategies you can try to help alleviate symptoms and promote healing. Here are some tips:
-
Follow a Skincare Routine: Establish a gentle skincare routine that includes regular bathing with mild, fragrance-free cleansers, followed by the application of a moisturizer. Moisturizing the skin at least twice a day helps to lock in moisture and reduce dryness.
-
Avoid Triggers: Identify and avoid triggers that worsen your atopic dermatitis symptoms. Common triggers include certain fabrics, harsh detergents, fragrances, and certain foods. Keeping a diary to track your symptoms can help identify potential triggers.
-
Use Protective Clothing: Wear loose-fitting, breathable clothing made from soft fabrics like cotton. Avoid wool or synthetic materials that may irritate the skin. Additionally, consider using cotton gloves or mittens to prevent scratching during sleep.
-
Moisturize Regularly: Keep your skin well-hydrated by applying moisturizers throughout the day, especially after bathing or washing your hands. Look for moisturizers that are fragrance-free and designed for sensitive skin.
-
Manage Stress: Stress can trigger or worsen atopic dermatitis symptoms. Practice stress-management techniques such as deep breathing exercises, meditation, yoga, or engaging in activities you enjoy.
-
Seek Medical Advice: If your atopic dermatitis symptoms persist or worsen despite home remedies, it is important to consult with a healthcare professional or dermatologist. They can provide a proper diagnosis, recommend appropriate treatments, and help develop a personalized management plan for your condition.
It is important to remember that atopic dermatitis varies from person to person, and what works for one individual may not work for another. A comprehensive approach that combines home remedies with medical guidance is often the most effective way to manage and reduce symptoms of atopic dermatitis.
Oatmeal Bath
An oatmeal bath is a popular home remedy for soothing the symptoms of atopic dermatitis. Oatmeal contains compounds called avenanthramides, which have anti-inflammatory properties and can help alleviate itching, redness, and irritation. Here’s how to take an oatmeal bath:
-
Grind the Oats: Start by grinding plain, unflavored oats into a fine powder using a blender or food processor. Make sure the oats are finely ground to enhance their soothing properties.
-
Prepare the Bath: Fill your bathtub with lukewarm water. Avoid using hot water as it can further dry out the skin and worsen eczema symptoms. Add the ground oatmeal to the running water and mix well to ensure it is evenly dispersed.
-
Soak in the Bath: Immerse yourself in the oatmeal-infused water and soak for about 15 to 20 minutes. Gently massage the affected areas of your skin to help the oatmeal soothe and moisturize the skin.
-
Pat Dry and Moisturize: After the bath, pat your skin dry with a soft towel, leaving some moisture on the skin. Immediately apply a gentle, fragrance-free moisturizer to lock in the hydration and further soothe the skin.
Oatmeal baths can provide temporary relief from itching, redness, and inflammation associated with atopic dermatitis. However, it is important to note that they may not be a long-term solution and should be used in conjunction with other treatments recommended by a healthcare professional.
Coconut Oil
Coconut oil is a natural moisturizer that can be beneficial for individuals with atopic dermatitis. It contains fatty acids that help hydrate the skin, reduce dryness, and soothe itching. Here’s how to use coconut oil for atopic dermatitis:
-
Choose Virgin Coconut Oil: Opt for organic, virgin coconut oil that is free from additives or fragrances. This type of coconut oil retains its natural properties and is less likely to cause irritation.
-
Test for Sensitivity: Before applying coconut oil to the affected areas, perform a patch test on a small area of skin. This helps ensure that you do not have an adverse reaction to the oil.
-
Apply to Damp Skin: After bathing or showering, when your skin is still damp, take a small amount of coconut oil and gently massage it into the affected areas. Allow the oil to absorb into the skin.
-
Repeat Regularly: Apply coconut oil to the affected areas at least twice a day or as needed to keep the skin moisturized and relieve itching. Consistent application is key to maintaining the skin’s hydration and barrier function.
Coconut oil can provide temporary relief from dryness and itching associated with atopic dermatitis. However, it is important to note that its effectiveness may vary among individuals, and it may not work for everyone. If you have any concerns or if your symptoms worsen, consult with a healthcare professional or dermatologist.
Apple Cider Vinegar
Apple cider vinegar is a natural remedy that some individuals use to alleviate the symptoms of atopic dermatitis. It has antimicrobial and anti-inflammatory properties that may help reduce redness, itching, and irritation. Here’s how to use apple cider vinegar for atopic dermatitis:
-
Dilute the Vinegar: Mix equal parts of raw, unfiltered apple cider vinegar and water. This dilution helps prevent any potential skin irritation that may occur when using undiluted vinegar.
-
Apply with a Compress: Soak a clean cloth or cotton ball in the diluted apple cider vinegar solution. Gently apply the compress to the affected areas of the skin. Leave it on for a few minutes before rinsing it off with lukewarm water.
-
Moisturize Afterward: After rinsing off the vinegar solution, pat your skin dry and apply a moisturizer to help replenish moisture and soothe the skin.
-
Use with Caution: Apple cider vinegar may not be suitable for everyone, especially those with sensitive skin or open wounds. It is important to perform a patch test before applying it to larger areas and to discontinue use if any adverse reactions occur.
While some individuals may find relief from using apple cider vinegar, it is important to note that scientific evidence supporting its effectiveness in treating atopic dermatitis is limited. It is advisable to consult with a healthcare professional or dermatologist before using apple cider vinegar as a remedy for atopic dermatitis.
What is the general management of eczema? :
The general management of atopic dermatitis involves a multifaceted approach that focuses on controlling symptoms, preventing flare-ups, and maintaining the overall health of the skin. Here are some key strategies for managing atopic dermatitis:
-
Skincare Routine: Establish a regular skincare routine that includes gentle cleansing with mild, fragrance-free products and regular moisturization with emollients. Avoid harsh soaps, hot water, and excessive scrubbing, as these can further irritate the skin.
-
Trigger Avoidance: Identify and avoid triggers that worsen your atopic dermatitis symptoms. Common triggers include certain fabrics, harsh detergents, fragrances, stress, and allergens. Keeping a diary to track your symptoms can help identify potential triggers.
-
Moisturize Regularly: Apply emollients or moisturizers to the skin at least twice a day, or as directed by a healthcare professional. This helps to keep the skin hydrated, reduce dryness, and maintain the skin barrier function.
-
Medications: In cases of moderate to severe atopic dermatitis, healthcare professionals may prescribe topical corticosteroids or other medications to reduce inflammation and control symptoms. These medications should be used as directed and under the supervision of a healthcare professional.
-
Lifestyle Modifications: Make necessary lifestyle changes to support skin health. This may include wearing soft, breathable clothing made from natural fibers, avoiding excessive sweating, managing stress levels, and practicing good hygiene.
-
Regular Follow-up: It is important to have regular follow-up appointments with a healthcare professional or dermatologist to monitor your condition, adjust treatment plans if necessary, and address any concerns or questions you may have.
By implementing these general management strategies, individuals with atopic dermatitis can effectively control symptoms, reduce the frequency and severity of flare-ups, and improve their overall quality of life. However, it is essential to work closely with a healthcare professional to develop a personalized management plan tailored to your specific needs.
Eczema Flare-ups
Atopic dermatitis, commonly known as eczema, is characterized by periods of flare-ups and remission. Eczema flare-ups refer to the sudden worsening of symptoms, including redness, itching, dryness, and inflammation. These flare-ups can be triggered by various factors such as allergens, irritants, changes in weather, stress, and certain foods. During a flare-up, the skin becomes more sensitive and prone to further irritation and infection.
To manage eczema flare-ups, it is important to identify and avoid triggers. This may involve making lifestyle changes such as using gentle skincare products, avoiding harsh chemicals, wearing loose-fitting clothing made from natural fibers, and maintaining a consistent skincare routine. Additionally, regular moisturization is crucial to keep the skin hydrated and prevent excessive dryness.
In some cases, healthcare professionals may recommend the use of topical corticosteroids or other prescribed medications to reduce inflammation and control symptoms during flare-ups. These medications should be used as directed and for the recommended duration. It is important to follow the guidance of a healthcare professional to ensure safe and effective use.
Emollients
Emollients play a vital role in the management of atopic dermatitis. These moisturizing products help restore and maintain the skin’s natural barrier function, preventing moisture loss and reducing dryness. Emollients come in various forms such as creams, lotions, ointments, and oils. They are typically applied to the skin multiple times a day, especially after bathing, to lock in moisture.
When choosing emollients for atopic dermatitis, it is important to opt for products that are fragrance-free, hypoallergenic, and specifically formulated for sensitive skin. Thick and greasy ointments are often preferred for individuals with severe dryness, while lighter lotions or creams may be suitable for milder cases. Emollients should be applied gently in the direction of hair growth to avoid further skin irritation.
Regular and consistent use of emollients is key to managing atopic dermatitis and preventing flare-ups. They not only provide immediate relief from dryness and itching but also help improve the skin’s overall health and resilience over time.
Wet Wrap Therapy
Wet wrap therapy is a technique used to provide intense hydration and relieve symptoms during severe atopic dermatitis flare-ups. It involves applying a layer of emollient to the affected areas and then wrapping them with dampened bandages or clothing. The dampness helps to enhance the absorption of the emollient, soothe itching, and calm inflammation.
To perform wet wrap therapy, start by taking a lukewarm bath or shower to hydrate the skin. Pat the skin dry gently, leaving it slightly damp. Next, apply a liberal amount of emollient to the affected areas. Then, dampen a bandage or piece of clothing with warm water and wrap it around the treated areas. It is important to ensure that the wrap is snug but not too tight, allowing for comfortable movement.
Wet wrap therapy can be left on for a few hours or overnight, depending on the severity of the flare-up and the guidance of a healthcare professional. After removing the wrap, gently pat the skin dry and apply a moisturizer to lock in the hydration.
It is important to note that wet wrap therapy should be used under the guidance of a healthcare professional, as it may not be suitable for everyone and can cause discomfort or skin irritation if not performed correctly. It is best to consult with a healthcare professional to determine if wet wrap therapy is appropriate for your specific condition and to receive proper instructions on its application.
Our Related Links
Conclusion
In conclusion, atopic dermatitis, commonly known as eczema, is a chronic skin condition characterized by dryness, itching, inflammation, and rash. It can significantly impact the quality of life for those affected, causing discomfort, sleep disturbances, and emotional distress. While the exact cause of atopic dermatitis remains unknown, it is believed to involve a combination of genetic and environmental factors.
Managing atopic dermatitis requires a comprehensive approach that includes skincare routines, trigger avoidance, regular moisturization, and, in some cases, medication. Establishing a gentle skincare routine, using fragrance-free products, and regularly moisturizing the skin are essential steps to maintain skin health and reduce the frequency of flare-ups. Identifying and avoiding triggers such as certain fabrics, detergents, stress, and allergens can help prevent exacerbation of symptoms.
Additionally, seeking medical advice and following the guidance of healthcare professionals is crucial in managing atopic dermatitis effectively. Healthcare professionals may prescribe topical corticosteroids or other medications to reduce inflammation and control symptoms during flare-ups. They can also provide personalized recommendations and treatment plans based on the severity and individual needs of each patient.
While there is no cure for atopic dermatitis, with proper management and care, individuals can achieve significant improvement in symptoms and enjoy a better quality of life. It is important to remember that what works for one person may not work for another, so it may require some trial and error to find the most effective management strategies.
Q : Can atopic dermatitis be cured?
A : Atopic dermatitis is a chronic condition, and there is currently no known cure. However, with proper management and care, symptoms can be controlled and minimized, allowing individuals to lead a better quality of life.
Q : What triggers atopic dermatitis flare-ups?
A : Triggers for atopic dermatitis flare-ups can vary from person to person. Common triggers include certain fabrics, harsh detergents, fragrances, stress, allergens, and weather changes. Identifying and avoiding triggers is an important part of managing the condition.
Q : Are there any natural remedies for atopic dermatitis?
A : While there are various natural remedies that some individuals find helpful in managing atopic dermatitis, it is important to note that their effectiveness may vary. Natural remedies such as oatmeal baths, coconut oil, and apple cider vinegar can provide relief for some people, but it is advisable to consult with a healthcare professional before trying any new remedies.
Q : Is atopic dermatitis contagious?
A : No, atopic dermatitis is not contagious. It is a non-infectious condition that results from a combination of genetic and environmental factors.
Q : Can stress worsen atopic dermatitis symptoms?
A : Yes, stress can trigger or worsen atopic dermatitis symptoms. Managing stress through relaxation techniques, exercise, and seeking support can help reduce flare-ups and improve symptom control.
Mor Links


