Banishing Acne for Good: 5 Best , Authentic & Potent Strategies to Reclaim Clear Skin

Overview
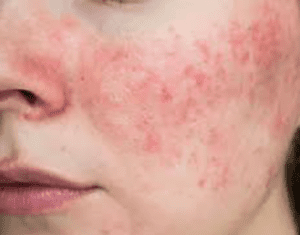
Acne is a common skin condition that affects millions of people worldwide. It occurs when hair follicles become clogged with oil and dead skin cells, leading to the formation of pimples, blackheads, and whiteheads. Acne can range from mild to severe and may cause physical discomfort as well as emotional distress due to its impact on appearance. While it is most prevalent during adolescence, acne can persist into adulthood for some individuals. Effective treatments and skincare routines can help manage and reduce acne symptoms, promoting clearer and healthier skin.
5 Potent Strategies to Reclaim Clear Skin
-
Consistent Cleansing Routine: Adopt a gentle and consistent cleansing routine to remove excess oil, dirt, and dead skin cells from your face. Use a mild cleanser twice daily to avoid over-drying the skin, which can trigger more oil production.
-
Topical Treatments: Incorporate over-the-counter or prescription topical treatments containing ingredients like benzoyl peroxide, salicylic acid, or retinoids. These potent ingredients can help unclog pores, reduce inflammation, and promote skin cell turnover.
-
Hydration and Diet: Stay well-hydrated and maintain a balanced diet rich in fruits, vegetables, and whole grains. A healthy diet can support skin health and reduce inflammation.
-
Hands Off Approach: Avoid picking, popping, or squeezing acne lesions, as it can worsen the condition and lead to scarring. Keep hands away from the face and avoid touching the affected areas.
-
Regular Exfoliation: Exfoliate the skin once or twice a week with a gentle scrub to remove dead skin cells and promote a smoother complexion. However, be cautious not to over-exfoliate, as it can irritate the skin.
Remember that acne treatment can vary based on individual skin types and severity, so consulting a dermatologist is essential for personalized care and guidance. With dedication to these potent strategies, you can take significant steps toward reclaiming clear and healthy skin.
Introduction:
Acne is a common skin condition that affects millions of people worldwide, regardless of age or gender. It manifests as various types of blemishes on the skin, such as pimples, blackheads, whiteheads, and even more severe forms like cysts or nodules. These unsightly skin imperfections typically appear on the face, neck, chest, back, and shoulders. While acne is most commonly associated with the adolescent years, it can persist into adulthood and even emerge for the first time in later stages of life.

The development of acne is primarily linked to hormonal changes within the body. During puberty, the body undergoes significant hormonal fluctuations, particularly an increase in androgens, which stimulate the sebaceous glands in the skin. These glands produce sebum, an oily substance that helps lubricate and protect the skin. However, when an excess of sebum is produced or when dead skin cells block the hair follicles, it can lead to the formation of acne.
Acne not only affects the physical appearance of individuals but also has a profound impact on their emotional well-being. It can cause feelings of self-consciousness, low self-esteem, and even social withdrawal. Understanding the causes, types, and treatment options for acne is crucial in order to effectively manage and address this common skin condition. In the following sections, we will delve deeper into the different types of acne, explore the underlying triggers, discuss effective treatment options, and provide valuable tips for prevention and skincare. By gaining a comprehensive understanding of acne, you will be better equipped to navigate this condition and maintain healthy, clear skin.
What are the 4 main causes of acne? :
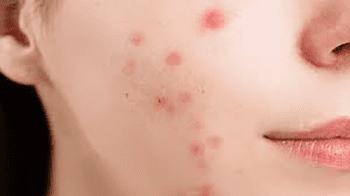
The four main causes of acne include:
-
Excessive sebum production: Overactive sebaceous glands produce an excess of sebum, leading to clogged pores and acne formation.
-
Buildup of dead skin cells: When dead skin cells accumulate and mix with sebum, they can block the hair follicles, resulting in the formation of blackheads and whiteheads.
-
Bacterial growth: The presence of Propionibacterium acnes, a bacterium naturally found on the skin, can multiply in clogged pores and cause inflammation, leading to acne breakouts.
-
Inflammation: Inflammatory responses triggered by factors like hormonal changes, bacteria, or irritation can contribute to the development of inflamed acne lesions, such as papules, pustules, cysts, or nodules.
Understanding these underlying causes of acne is essential for effective treatment and prevention strategies. By addressing these factors, individuals can adopt appropriate skincare routines, make lifestyle modifications, and seek professional guidance to manage and minimize the occurrence of acne breakouts.
Hormonal Acne:
Hormonal acne is closely associated with fluctuations in hormone levels, particularly during puberty, the menstrual cycle, and pregnancy. Increased androgen production stimulates the sebaceous glands, leading to excessive sebum production. This excess sebum, along with dead skin cells, can clog the hair follicles and result in the formation of acne. Hormonal acne often presents as deep, painful cysts or nodules that are difficult to treat with topical solutions alone. Consulting a dermatologist for effective hormonal acne management is recommended, as hormonal therapies or oral medications may be prescribed to balance hormone levels and reduce acne breakouts.
Diet and Acne:
While there is no definitive evidence linking specific foods to acne, certain dietary factors may influence its development and severity. Diets high in refined carbohydrates, such as sugary foods and beverages, white bread, and processed snacks, have been associated with increased insulin levels. Elevated insulin levels can trigger inflammation and stimulate the production of sebum, contributing to acne formation. Additionally, dairy products and foods with a high glycemic index (such as sugary drinks and snacks) have been suggested to exacerbate acne in some individuals. However, the impact of diet on acne can vary among individuals, and it is important to maintain a balanced diet and observe how specific foods may affect your skin.
Stress and Acne:
Stress does not directly cause acne, but it can worsen existing acne or trigger flare-ups. During times of stress, the body produces higher levels of stress hormones like cortisol, which can increase sebum production and inflammation in the skin. Moreover, stress can disrupt healthy skincare routines, leading to neglect of proper cleansing, increased touching of the face, or unhealthy coping mechanisms like excessive consumption of comfort foods or tobacco use, which can all contribute to acne development. Managing stress through relaxation techniques, regular exercise, and adopting healthy coping mechanisms can help minimize its impact on acne.
Genetic Factors:

Genetics play a role in acne susceptibility. If your parents or close relatives had a history of acne, you may be more likely to develop it as well. Genetic factors can influence the size and activity of sebaceous glands, the skin’s ability to shed dead skin cells, and the body’s response to inflammation. While genetic predisposition does not guarantee acne development, it can increase the risk. Understanding your genetic predisposition can help you take proactive measures to manage and prevent acne, such as adopting a consistent skincare routine and seeking professional treatment when needed.
What are the symptoms of acne? :
The symptoms of acne can vary depending on the severity of the condition. Common symptoms include the presence of:

- Blackheads: Open comedones that appear as small, dark bumps on the skin’s surface.
- Whiteheads: Closed comedones that are small, flesh-colored bumps beneath the skin’s surface.
- Papules: Small, raised, red bumps that may be tender to touch.
- Pustules: Red, inflamed bumps with a white or yellow center filled with pus.
- Cysts or nodules: Large, painful, deep-seated bumps beneath the skin that can cause scarring.
In addition to these physical symptoms, acne can also lead to emotional distress, low self-esteem, and social withdrawal. It is important to seek professional guidance and adopt appropriate treatment methods to manage acne effectively and minimize its impact on both physical and mental well-being.
Cystic Acne:
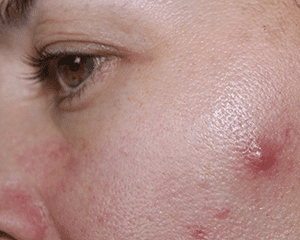
Cystic acne is a severe form of acne that results from deep inflammation and infection in the skin. It is characterized by the development of large, painful cysts or nodules beneath the surface of the skin. Cystic acne is often resistant to topical treatments and can lead to significant scarring if not properly managed. The lesions associated with cystic acne are typically red, swollen, and filled with pus. It is crucial to consult a dermatologist for appropriate treatment options, which may include oral medications such as antibiotics, isotretinoin, or hormonal therapies to address the underlying causes of cystic acne and prevent long-term scarring.
Acne Scars:

Acne scars are the result of inflammation and tissue damage caused by severe acne lesions. When acne penetrates deep into the skin, it can damage the collagen fibers, leaving behind permanent scars. There are different types of acne scars, including ice pick scars (deep and narrow), boxcar scars (shallow with defined edges), and rolling scars (wave-like or undulating appearance). The treatment of acne scars depends on their type and severity. Options may include laser therapy, chemical peels, microneedling, dermal fillers, or surgical techniques. It is essential to seek professional advice from a dermatologist or a skincare specialist to determine the most suitable treatment approach for acne scars.
What is the diagnostic for acne? :
The diagnosis of acne is primarily based on a visual examination of the skin and the presence of characteristic acne lesions. In some cases, additional diagnostic tests may be performed to rule out other skin conditions or hormonal imbalances that can contribute to acne development. These tests may include blood tests to assess hormone levels or skin swabs to identify specific bacteria. However, in most cases, a dermatologist can diagnose acne based on a thorough evaluation of the skin’s appearance and the individual’s medical history.
Types of Acne:
There are several types of acne, each characterized by different types of lesions and levels of severity:
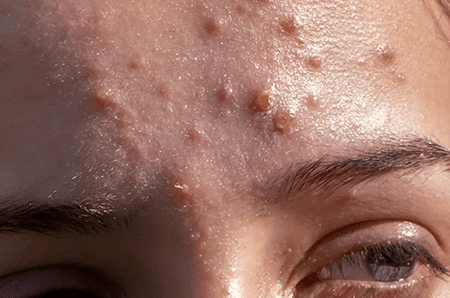
-
Comedonal Acne: This type of acne is characterized by the presence of comedones, which can be open (blackheads) or closed (whiteheads). Comedonal acne is often mild and can be effectively treated with topical retinoids or salicylic acid.
-
Inflammatory Acne: Inflammatory acne includes papules, pustules, and nodules. Papules are small, red bumps, while pustules are inflamed bumps with a white or yellow center filled with pus. Nodules are large, painful, deep-seated bumps beneath the skin. Inflammatory acne requires more aggressive treatment, such as topical or oral medications, to reduce inflammation and prevent scarring.
-
Cystic Acne: Cystic acne is the most severe form of acne, characterized by deep, painful cysts or nodules beneath the skin. It is often resistant to topical treatments and can lead to significant scarring. Treatment for cystic acne usually involves oral medications, such as isotretinoin, to address the underlying causes and prevent long-term scarring.
Acne Symptoms:
Common symptoms of acne include:
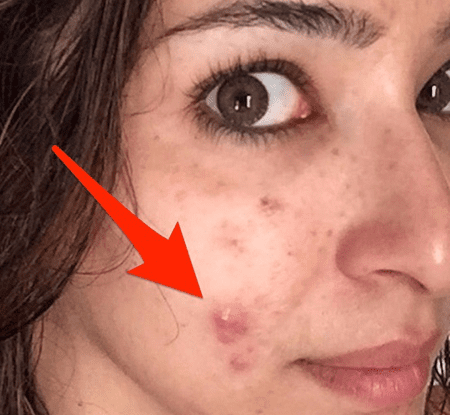
- Presence of blackheads, whiteheads, papules, pustules, or cysts on the skin.
- Redness and inflammation around the acne lesions.
- Pain or tenderness in the affected areas.
- Oily skin or an increase in oiliness.
- Scarring or hyperpigmentation after the acne lesions heal.
The severity of symptoms can vary from mild to severe, and it is important to seek professional guidance for an accurate diagnosis and appropriate treatment.
Acne Skin Analysis:

Acne skin analysis involves examining the skin to determine the type and severity of acne and develop a customized treatment plan. A dermatologist or skincare professional will assess the skin’s condition, identify the types of lesions present, evaluate the extent of inflammation, and examine any scarring or hyperpigmentation. This analysis helps determine the appropriate treatment approach, which may include topical medications, oral medications, lifestyle modifications, or procedural interventions like chemical peels or laser therapy.
Can acne be preventable? :
While some skin diseases may have genetic or underlying medical causes that make them difficult to prevent entirely, adopting preventive measures can significantly reduce the risk of developing or worsening skin conditions. By practicing good skincare habits, avoiding triggers, and maintaining a healthy lifestyle, you can help minimize the likelihood and severity of certain skin diseases. It’s important to consult with a dermatologist or healthcare professional for personalized advice and guidance based on your specific condition.
Skincare Routine for Managing Skin Disease:
Developing a consistent skincare routine is crucial for managing skin diseases effectively. Whether you’re dealing with acne, psoriasis, eczema, or any other skin condition, a proper skincare routine can help alleviate symptoms and promote healthier skin. Here are key steps to include in your skincare routine:
-
Gentle Cleansing: Use a mild, non-irritating cleanser to remove impurities from the skin without stripping away natural oils. Avoid harsh cleansers that can exacerbate skin conditions. Gently massage the cleanser onto your skin, then rinse thoroughly with lukewarm water.
-
Moisturizing: Moisturizing is essential to maintain skin hydration and prevent dryness, which can worsen many skin diseases. Choose a moisturizer specifically formulated for your skin type and condition. Look for ingredients like ceramides, hyaluronic acid, or shea butter that help lock in moisture.
-
Targeted Treatments: Depending on the specific skin disease, you may need to incorporate targeted treatments into your routine. These may include topical medications prescribed by a dermatologist, such as corticosteroids, retinoids, or antimicrobial creams. Follow your healthcare provider’s instructions for application.
-
Sun Protection: Protecting your skin from the sun’s harmful UV rays is crucial, as many skin diseases can worsen with sun exposure. Apply a broad-spectrum sunscreen with SPF 30 or higher before going outdoors, and reapply every two hours. Additionally, wear protective clothing and seek shade during peak sun hours.
Skin Disease Prevention Tips:
While it may not always be possible to prevent skin diseases entirely, there are steps you can take to minimize the risk of developing or worsening certain conditions. Here are some prevention tips:
-
Practice Good Hygiene: Maintain proper hygiene by washing your skin regularly with gentle cleansers. Avoid using harsh soaps or excessive scrubbing, as they can disrupt the skin’s natural barrier and trigger inflammation.
-
Avoid Triggers: Identify and avoid triggers that exacerbate your skin disease. These triggers can vary depending on the condition but may include certain foods, environmental factors (such as pollen or pet dander), stress, or specific skincare products. Keeping a journal to track flare-ups can help identify potential triggers.
-
Protect Your Skin: Shield your skin from harsh environmental factors by wearing appropriate clothing, such as long sleeves, hats, or gloves. This can help protect against irritants, allergens, or extreme temperatures that can worsen skin conditions.
-
Manage Stress: Stress can aggravate many skin diseases, so it’s important to find healthy ways to manage stress levels. Engage in relaxation techniques, exercise regularly, get enough sleep, and seek support from friends, family, or professionals when needed.
What are the top 3 best acne treatments? :
Determining the best treatment for a skin disease depends on various factors, including the specific condition, its severity, and individual response. However, here are three commonly recommended treatments for managing skin diseases:
-
Topical Corticosteroids: Corticosteroids are widely used and highly effective in reducing inflammation and managing symptoms in many skin diseases. They provide rapid relief from itching, redness, and irritation.
-
Retinoids: Retinoids are versatile and effective in treating various skin diseases, including acne, psoriasis, and photoaging. They help regulate cell turnover, unclog pores, and reduce inflammation, resulting in improved skin appearance.
-
Biologic Medications: Biologic medications have revolutionized the treatment of certain autoimmune skin diseases. They target specific molecules involved in the immune response, providing targeted relief from inflammation and controlling symptoms.
It’s important to consult with a dermatologist or healthcare professional to determine the most suitable treatment for your specific skin disease, as they can provide personalized recommendations based on your condition, medical history, and individual needs.
Topical Treatments for Managing Skin Disease:
Topical treatments are commonly used for managing various skin diseases and can help alleviate symptoms and promote healing. These treatments are applied directly to the skin and come in various forms, such as creams, gels, lotions, or ointments. Here are some commonly used topical treatments:
-
Corticosteroids: Corticosteroid creams or ointments are effective in reducing inflammation and itching associated with many skin diseases. They work by suppressing the immune response and can provide relief from symptoms like redness, swelling, and irritation.
-
Retinoids: Retinoids are derivatives of vitamin A and are commonly used for treating skin conditions like acne, psoriasis, and photoaging. They work by promoting cell turnover, unclogging pores, and reducing inflammation. Retinoids can be available as prescription medications or over-the-counter formulations.
-
Topical Antibiotics: Antibiotics in topical form, such as erythromycin or clindamycin, are often prescribed to manage skin diseases characterized by bacterial infections or inflammation. They help control bacterial growth, reduce redness, and promote healing.
-
Calcineurin Inhibitors: Calcineurin inhibitors, like tacrolimus or pimecrolimus, are commonly used for treating inflammatory skin conditions such as eczema or atopic dermatitis. They work by inhibiting the immune response and reducing inflammation.
Prescription Medications for Skin Disease:
For more severe or persistent skin diseases, prescription medications may be necessary to manage symptoms effectively. These medications are typically prescribed by a dermatologist or healthcare professional. Here are some commonly used prescription medications:
-
Oral Steroids: Oral corticosteroids, such as prednisone, are prescribed for severe inflammation or flare-ups of certain skin diseases like severe eczema or autoimmune conditions. They provide systemic relief by reducing inflammation throughout the body.
-
Immunosuppressants: Immunosuppressive medications, such as methotrexate or cyclosporine, are used for severe cases of autoimmune skin diseases like psoriasis or pemphigus. These medications suppress the immune system to control the immune response that triggers the skin disease.
-
Biologics: Biologic medications, such as adalimumab or ustekinumab, are a newer class of drugs used to treat certain autoimmune skin diseases. They target specific molecules involved in the immune response, reducing inflammation and controlling symptoms.
-
Antihistamines: Antihistamines, such as cetirizine or fexofenadine, are prescribed to manage allergic skin conditions like urticaria or allergic contact dermatitis. They help relieve itching, redness, and swelling by blocking the effects of histamine in the body.
Natural Remedies for Skin Disease:
In addition to conventional treatments, some individuals may seek natural remedies to manage skin diseases. It’s important to note that natural remedies may not work for everyone, and their effectiveness can vary. Here are some natural remedies that may be beneficial for certain skin conditions:
-
Aloe Vera: Aloe vera gel is known for its soothing and anti-inflammatory properties. It can be applied topically to alleviate itching, redness, and irritation associated with skin diseases.
-
Tea Tree Oil: Tea tree oil has antimicrobial and anti-inflammatory properties, making it a popular choice for managing acne, psoriasis, or fungal infections. However, it should be used with caution, as it can cause skin irritation in some individuals.
-
Oatmeal: Oatmeal baths or oatmeal-based products can help soothe itching and inflammation in conditions like eczema or allergic skin reactions. It forms a protective barrier on the skin, reducing moisture loss and promoting healing.
-
Coconut Oil: Coconut oil is a natural moisturizer that can be beneficial for dry skin conditions. It helps hydrate the skin and may provide relief from symptoms like itching or flaking.
How can I get rid of acne by lifestyle? :
Lifestyle changes can play a significant role in managing skin diseases and improving skin health. While individual results may vary, here are some lifestyle modifications that can contribute to the management of skin diseases:
-
Maintain a Healthy Skincare Routine: Establish a consistent skincare routine that includes gentle cleansing, moisturizing, and the use of appropriate products for your skin type and condition. Avoid harsh chemicals or abrasive scrubs that can irritate the skin.
-
Follow a Balanced Diet: Adopt a balanced diet that includes fruits, vegetables, whole grains, lean proteins, and healthy fats. These provide essential nutrients and antioxidants that support overall skin health.
-
Practice Stress Management: Chronic stress can worsen certain skin diseases. Incorporate stress management techniques such as exercise, meditation, deep breathing exercises, or engaging in activities that promote relaxation.
-
Get Sufficient Sleep: A good night’s sleep is essential for skin repair and rejuvenation. Aim for 7-9 hours of quality sleep each night to support skin health and overall well-being.
-
Protect Your Skin: Shield your skin from harmful ultraviolet (UV) rays by using sunscreen with a broad-spectrum SPF, wearing protective clothing, and seeking shade during peak sun hours. UV exposure can worsen certain skin diseases and accelerate aging.
While lifestyle changes can contribute to managing skin diseases, it’s important to consult with a dermatologist or healthcare professional for an accurate diagnosis and personalized treatment plan. They can provide tailored advice and recommend specific lifestyle modifications that align with your condition and individual needs.
Acne-Friendly Diet: Promoting Skin Health through Nutrition
Maintaining a healthy diet is important for overall well-being, and it can also play a role in managing certain skin diseases. While there isn’t a specific “acne diet,” making certain dietary choices can support skin health and potentially minimize symptoms of skin diseases. Here are some dietary recommendations for promoting healthy skin:
-
Eat a Balanced Diet: Opt for a well-rounded diet that includes plenty of fruits, vegetables, whole grains, lean proteins, and healthy fats. These provide essential nutrients, vitamins, and antioxidants that contribute to overall skin health.
-
Limit Processed Foods and Sugar: Highly processed foods, sugary snacks, and beverages can potentially worsen skin conditions by triggering inflammation and increasing oil production. Limiting the intake of these foods and opting for whole, unprocessed options can be beneficial.
-
Stay Hydrated: Proper hydration is important for maintaining healthy skin. Drinking an adequate amount of water helps flush out toxins and keeps the skin hydrated and supple. Aim for at least eight glasses of water per day.
-
Consider Omega-3 Fatty Acids: Omega-3 fatty acids, found in fatty fish like salmon, walnuts, and chia seeds, have anti-inflammatory properties and can help reduce inflammation in the body, potentially benefiting certain skin diseases.
While diet alone may not completely cure skin diseases, adopting a balanced and skin-friendly diet can support overall skin health and potentially contribute to the management of symptoms.
Exercise and Skin Disease: The Connection and Benefits
Regular physical activity has numerous health benefits, and it can also have positive effects on certain skin diseases. Exercise promotes blood circulation, reduces stress, and supports overall well-being, which can indirectly benefit the skin. Here’s how exercise can contribute to managing skin diseases:
-
Improved Blood Circulation: Exercise increases blood flow, delivering oxygen and nutrients to the skin cells. This improved circulation can enhance the skin’s overall health and appearance.
-
Stress Reduction: Exercise is known to reduce stress levels by releasing endorphins, also known as “feel-good” hormones. Since stress can exacerbate certain skin diseases, engaging in regular physical activity can help manage stress and potentially minimize flare-ups.
-
Enhanced Immune Function: Regular exercise strengthens the immune system, which plays a crucial role in managing various skin diseases. A healthy immune system can better fight off infections and reduce inflammation in the body.
-
Detoxification: Sweating during exercise helps eliminate toxins from the body. This natural detoxification process can potentially benefit skin conditions by reducing the accumulation of impurities.
However, it’s important to note that excessive sweating or friction from tight-fitting workout clothes can potentially irritate the skin or worsen certain skin diseases. It’s recommended to shower and change into clean, loose-fitting clothing after exercising to maintain skin hygiene.
Acne and Self-Esteem: Nurturing a Positive Body Image
Skin diseases, including acne, can have a significant impact on an individual’s self-esteem and body image. The visible nature of skin conditions may lead to self-consciousness, social withdrawal, and feelings of low self-worth. Here are some strategies for nurturing a positive body image:
-
Self-Care and Skincare: Prioritize self-care activities that make you feel good about yourself. Establish a skincare routine that focuses on gentle cleansing, moisturizing, and using products suitable for your skin type and condition.
-
Seek Professional Help: Consult with a dermatologist or healthcare professional who can provide appropriate treatment options for your skin disease. Addressing the condition can help alleviate symptoms and improve self-confidence.
-
Practice Positive Self-Talk: Be mindful of negative self-talk and challenge negative thoughts related to your skin disease. Focus on your strengths, accomplishments, and qualities that go beyond physical appearance.
-
Build a Supportive Network: Surround yourself with understanding and supportive individuals who value you for who you are beyond your skin condition. Engage in activities and relationships that bring you joy and boost your self-esteem.
Remember that self-esteem is not solely based on physical appearance. It’s important to cultivate self-acceptance, embrace your uniqueness, and prioritize overall well-being. Seeking support from professionals or support groups can be beneficial in managing the emotional impact of skin diseases and developing a positive body image.
What is an interesting fact about acne? :
Beyond the physical symptoms, skin diseases can have a significant impact on an individual’s mental well-being. The visible nature of skin conditions can lead to feelings of self-consciousness, social isolation, and emotional distress. It’s crucial to recognize the psychological aspects associated with skin diseases.
Research has shown that individuals with skin conditions may experience reduced self-esteem, body image concerns, anxiety, and depression. The emotional toll of living with skin diseases should not be overlooked or dismissed. Seeking emotional support from loved ones, joining support groups, or seeking counseling can provide valuable assistance in coping with the psychosocial challenges associated with skin diseases.
Promoting awareness, empathy, and understanding about the emotional impact of skin conditions can contribute to creating a supportive and inclusive environment for those affected.
Skin Disease Myths: Debunking Misconceptions about Skin Conditions
Skin diseases are often surrounded by numerous myths and misconceptions. These misunderstandings can lead to ineffective treatments or unnecessary anxiety. Here are a few common skin disease myths debunked:
-
Myth: Skin diseases are contagious. Fact: Many skin diseases are not contagious and cannot be transmitted from person to person through casual contact. Conditions like eczema, psoriasis, and rosacea are examples of non-contagious skin diseases. It’s important to understand that each skin condition has its own causes and modes of transmission, and not all skin diseases are contagious.
-
Myth: Skin diseases are always caused by poor hygiene. Fact: While maintaining good hygiene is important for overall skin health, not all skin diseases are caused by poor hygiene. Skin diseases can be influenced by various factors such as genetics, hormonal imbalances, immune system disorders, allergies, and environmental triggers. It’s crucial to consult with a dermatologist or healthcare professional to determine the underlying causes of specific skin conditions.
-
Myth: Exposure to sunlight is the best remedy for skin diseases. Fact: While sunlight can have some beneficial effects on certain skin conditions, such as psoriasis or vitiligo, excessive sun exposure can worsen other skin diseases. Sunburn, inflammation, and increased risk of skin cancer are potential risks associated with prolonged sun exposure. It’s important to seek professional advice and take necessary precautions when managing skin diseases.
-
Myth: Only topical treatments can effectively manage skin diseases. Fact: While topical treatments can be an integral part of managing many skin diseases, they may not be the sole solution for every condition. Some skin diseases require a multidimensional approach that may include lifestyle modifications, systemic medications, phototherapy, or other specialized treatments. It’s essential to work closely with a healthcare professional to develop a comprehensive treatment plan.
Home Remedies for Skin Conditions: Natural Approaches
Many individuals seek natural remedies to complement their treatment plans for skin conditions. While home remedies may not replace medical advice or prescribed treatments, they can offer temporary relief or support skin health. Here are a few commonly used home remedies:
-
Oatmeal: Oatmeal has soothing properties and can provide relief for itching and inflammation associated with certain skin conditions. Adding colloidal oatmeal to a lukewarm bath or applying an oatmeal paste directly to the affected area can help alleviate discomfort.
-
Aloe Vera: Aloe vera gel has cooling and moisturizing properties that can soothe irritated skin. Applying pure aloe vera gel to the affected area can provide relief from itching and inflammation.
-
Coconut Oil: Coconut oil contains fatty acids that help moisturize and protect the skin barrier. Applying virgin coconut oil to dry or inflamed skin can help retain moisture and reduce symptoms.
-
Chamomile: Chamomile has anti-inflammatory and calming properties that can benefit various skin conditions. Infusing chamomile tea bags in warm water and using the solution as a compress or adding chamomile essential oil to a carrier oil can help soothe the skin.
It’s important to note that individual responses to home remedies may vary, and some people may be sensitive to certain ingredients. It’s recommended to patch test any new remedy on a small area of the skin and discontinue use if any irritation or adverse reactions occur. Consulting with a dermatologist or healthcare professional is advisable to ensure proper diagnosis and guidance on suitable treatments.
Conclusion
In conclusion, skin diseases can significantly impact a person’s physical and emotional well-being. While each skin condition has its unique characteristics and causes, there are some common themes in managing and preventing skin diseases.
Maintaining a healthy lifestyle, including a balanced diet, regular exercise, and stress management, can help promote overall skin health. Following a consistent skincare routine tailored to the specific needs of the skin disease can also contribute to managing symptoms and preventing flare-ups.
When it comes to treatment, there are various options available, including topical treatments, prescription medications, and natural remedies. It’s essential to consult with a dermatologist or healthcare professional to determine the most suitable treatment approach based on the severity and specific characteristics of the skin disease.
Furthermore, debunking myths and misconceptions surrounding skin diseases is crucial to ensure accurate information and appropriate care. By raising awareness, fostering understanding, and providing support, we can create a more inclusive and compassionate environment for individuals living with skin diseases.
Q: 1. Can skin diseases be completely cured?
A: The treatment and management of skin diseases depend on the specific condition. While some skin diseases can be controlled and symptoms managed effectively, complete cures may not always be possible. Working closely with a dermatologist or healthcare professional can help develop a personalized treatment plan.
Q: 2. Are all skin diseases contagious?
A: No, not all skin diseases are contagious. Some skin diseases, such as eczema or psoriasis, are non-contagious and cannot be transmitted from person to person through casual contact. However, certain skin conditions, like fungal infections or certain types of rashes, can be contagious and require appropriate precautions.
Q: 3. Are natural remedies effective in treating skin diseases?
A: Natural remedies can provide temporary relief or support skin health in some cases, but their effectiveness varies depending on the skin disease and individual response. It’s important to consult with a dermatologist or healthcare professional before relying solely on natural remedies to ensure appropriate diagnosis and treatment.
Q: 4. Can lifestyle changes help in managing skin diseases?
A: Yes, certain lifestyle changes can contribute to managing and preventing skin diseases. Maintaining a healthy diet, engaging in regular physical activity, managing stress levels, and following a consistent skincare routine can support overall skin health and potentially reduce the frequency and severity of flare-ups.
Q: 5. Is it normal to feel self-conscious about having a skin disease?
A: It is normal to feel self-conscious about having a skin disease, as visible symptoms can impact one’s self-esteem and confidence. Seeking emotional support from loved ones, joining support groups, or seeking professional counseling can be beneficial in coping with the emotional aspects associated with skin diseases.
More Links
Acne Overview |
TREATMENT OF ACNE |
Know About Acne |
Acne Visual |