Glaucoma Uncovered: 5 best , Practical & Potent Strategies to Combat the Silent Thief
Overview
Glaucoma is a group of eye conditions that cause damage to the optic nerve, leading to vision loss or even blindness if left untreated. The main culprit behind glaucoma is increased pressure within the eye, known as intraocular pressure. The condition often develops slowly and may not show noticeable symptoms until later stages, which is why regular eye exams are crucial for early detection. While there is no cure for glaucoma, various treatments, such as eye drops, laser therapy, or surgery, can help manage the condition and prevent further vision deterioration. Early diagnosis and proper management are essential to preserve vision and reduce the risk of complications.
5 Potent Strategies to Combat the Silent Thief
-
Regular Eye Exams: Routine eye exams play a vital role in detecting glaucoma at its early stages when symptoms may not be apparent. Comprehensive eye check-ups help monitor intraocular pressure and assess the health of the optic nerve.
-
Medication Management: Glaucoma can often be controlled with the use of eye drops to lower intraocular pressure. Adhering to the prescribed medication schedule is crucial to prevent further damage to the optic nerve.
-
Lifestyle Modifications: Leading a healthy lifestyle can positively impact glaucoma management. Regular exercise, a balanced diet rich in antioxidants, and avoiding smoking can contribute to overall eye health.
-
Laser Treatment: Laser therapy, such as selective laser trabeculoplasty (SLT) or laser peripheral iridotomy (LPI), can be effective in lowering intraocular pressure and preventing further vision loss.
-
Surgery: In advanced cases, surgical procedures like trabeculectomy or shunt implantation may be recommended to reduce intraocular pressure and preserve vision.
It is important to note that glaucoma is a progressive condition, and early intervention is crucial for the best outcomes. Regular communication with an eye care professional and following their recommendations are essential to combat this silent thief and protect vision.
What is Glaucoma?
Glaucoma is a serious eye condition that affects millions of people worldwide. It is often referred to as the “silent thief of sight” because it can gradually damage the optic nerve and lead to irreversible vision loss if left untreated. Glaucoma is characterized by increased pressure within the eye, known as intraocular pressure, which can damage the optic nerve and affect the transmission of visual signals to the brain.
The exact cause of glaucoma is still not fully understood, but it is believed to be a combination of various factors, including genetics, age, and certain medical conditions. While anyone can develop glaucoma, certain individuals may be at a higher risk, such as those with a family history of the disease, older adults, and individuals with certain medical conditions like diabetes and high blood pressure.

Early detection and timely treatment are crucial in managing glaucoma and preventing further vision loss. Regular eye examinations, including measurements of intraocular pressure and comprehensive evaluations of the optic nerve, can help in the early detection of glaucoma. Treatment options for glaucoma may include eye drops, oral medications, laser therapy, or surgery, depending on the severity and progression of the condition.
It is important for individuals to be aware of the signs and symptoms of glaucoma, such as gradual loss of peripheral vision, tunnel vision, blurred vision, and eye pain. If any of these symptoms are experienced, it is essential to seek immediate medical attention from an eye care professional.
In conclusion, glaucoma is a sight-threatening condition that requires early detection, proper management, and ongoing care. By understanding the importance of regular eye examinations and being aware of the signs and symptoms, individuals can take proactive steps to protect their vision and maintain eye health.
What are the first signs that glaucoma is developing? :
Glaucoma is often referred to as the “silent thief of sight” because it can develop without obvious symptoms in its early stages. However, there are some initial signs that may indicate the possible development of glaucoma. These signs include increased intraocular pressure, optic nerve changes detected during an eye examination, changes in the visual field, and structural abnormalities of the eye.
Increased intraocular pressure is one of the primary risk factors for glaucoma development. Elevated pressure inside the eye can put strain on the optic nerve, potentially leading to damage over time. Regular eye examinations can measure intraocular pressure and identify any abnormalities that may indicate the presence of glaucoma.
Optic nerve changes detected during an eye examination can also be an early sign of glaucoma. Eye care professionals can evaluate the optic nerve using various imaging techniques and assess its condition. Changes in the appearance of the optic nerve, such as cupping or thinning, may indicate the presence of glaucoma.
Changes in the visual field, the area that can be seen without moving the eyes, can occur as glaucoma progresses. In the early stages, these changes may be subtle and go unnoticed by the individual. However, during comprehensive eye exams, eye care professionals can perform visual field tests to detect any abnormalities and monitor their progression over time.
Structural abnormalities of the eye, such as narrow angles or structural damage to the drainage system, can also increase the risk of glaucoma. These abnormalities can interfere with the normal flow of fluid within the eye, leading to increased intraocular pressure and potential optic nerve damage.
Regular comprehensive eye exams are crucial for detecting these early signs of glaucoma. By monitoring intraocular pressure, evaluating the optic nerve, assessing the visual field, and identifying any structural abnormalities, eye care professionals can diagnose glaucoma at an early stage. Early intervention and treatment can help preserve vision and prevent the progression of the disease.
Glaucoma Symptoms:
Glaucoma is a group of eye conditions that can result in damage to the optic nerve, leading to vision loss if left untreated. In the early stages, glaucoma often does not exhibit noticeable symptoms. However, as the condition progresses, certain symptoms may become evident. These symptoms include a gradual loss of peripheral vision, blurred vision, eye pain, redness, halos around lights, and in some cases, nausea and vomiting. It is crucial to recognize these symptoms and seek prompt medical attention to prevent further vision impairment.
Glaucoma is a complex eye condition that can be challenging to detect in its early stages. The optic nerve damage caused by glaucoma is typically irreversible, making early detection and treatment crucial for preserving vision. Regular eye examinations, especially for individuals at higher risk, such as those with a family history of glaucoma, are essential for early diagnosis.
In its early stages, glaucoma often progresses silently without causing noticeable symptoms. This can make it difficult for individuals to detect the condition without professional evaluation. Therefore, it is important to prioritize regular eye check-ups, even if no symptoms are present. An eye doctor can perform various tests to measure intraocular pressure, examine the optic nerve, and evaluate the visual field, enabling early detection of glaucoma.
Once glaucoma advances, certain symptoms may become more apparent. Gradual loss of peripheral vision is a common symptom experienced by individuals with glaucoma. This occurs because the optic nerve, responsible for transmitting visual information to the brain, becomes damaged over time. Additionally, blurred vision may occur due to increased pressure in the eye or optic nerve damage. Individuals with glaucoma may also experience eye pain, redness, and a sensation of pressure within the eye. Some individuals may even notice halos around lights, making it difficult to focus clearly. In severe cases, acute angle-closure glaucoma can cause episodes of nausea and vomiting.
To protect your vision and ensure early detection of glaucoma, it is crucial to schedule regular comprehensive eye exams. These exams allow eye care professionals to monitor intraocular pressure, evaluate the optic nerve, assess the visual field, and detect any signs of glaucoma. Early diagnosis and treatment can help prevent further vision loss and maintain the best possible eye health.
Open-Angle Glaucoma Symptoms:
Open-angle glaucoma is the most common form of glaucoma, accounting for approximately 90% of cases. Unlike some other types of glaucoma, open-angle glaucoma develops gradually over time. In its early stages, it may not exhibit noticeable symptoms, making it challenging to detect without regular eye examinations. This slow progression can result in significant vision loss before symptoms become apparent.
One of the primary symptoms experienced by individuals with open-angle glaucoma is a gradual loss of peripheral vision. Peripheral vision refers to the ability to see objects and movement outside the direct line of sight. As glaucoma progresses, the visual field narrows, and individuals may notice a reduction in their peripheral vision. However, since this occurs gradually, individuals may not be aware of the visual field loss until it reaches an advanced stage.
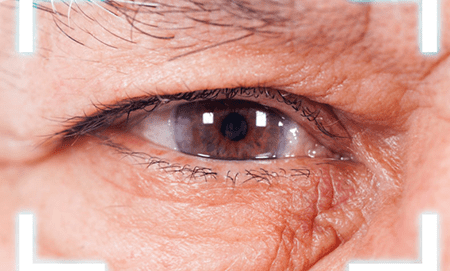
Another symptom associated with open-angle glaucoma is the presence of patchy blind spots in the visual field. These blind spots may start small and go unnoticed initially. However, over time, they can expand and merge, leading to significant visual impairment. The progression of open-angle glaucoma can also cause damage to the optic nerve, resulting in decreased clarity and contrast sensitivity. This can make it difficult to see details clearly and discern between different shades of light and dark.
It is important to note that open-angle glaucoma progresses slowly, and individuals may not experience symptoms until significant vision loss has occurred. Therefore, regular eye examinations are essential for early detection and treatment. By detecting open-angle glaucoma in its early stages, eye care professionals can implement strategies to manage intraocular pressure and preserve vision.
Acute Angle-Closure Glaucoma Symptoms:
Acute angle-closure glaucoma is a less common but more severe form of glaucoma. Unlike open-angle glaucoma, which develops gradually, acute angle-closure glaucoma manifests rapidly and requires immediate medical attention. This type of glaucoma occurs when the drainage angle of the eye becomes blocked, causing a sudden increase in intraocular pressure.
The symptoms of acute angle-closure glaucoma can be intense and alarming. One of the primary symptoms is sudden and severe eye pain. The pain is often described as a deep ache and may be accompanied by a feeling of pressure within the eye. Redness in the affected eye is also common and can be accompanied by blurred vision. Individuals may notice that their vision becomes hazy or that they have difficulty focusing clearly. Halos around lights, especially in low-light conditions, can also occur in acute angle-closure glaucoma. These halos may appear as colored rings or circles around light sources.

In some cases, acute angle-closure glaucoma can lead to additional symptoms such as nausea and vomiting. These symptoms are typically associated with severe increases in intraocular pressure. If left untreated, acute angle-closure glaucoma can cause irreversible damage to the optic nerve, leading to permanent vision loss.
It is important to seek immediate medical attention if you experience symptoms of acute angle-closure glaucoma. This condition requires emergency treatment to lower intraocular pressure and prevent further damage to the optic nerve. Prompt medical intervention can help preserve vision and prevent complications associated with acute angle-closure glaucoma.
What are the main causes of glaucoma? :
The main causes of glaucoma are primarily related to increased intraocular pressure and compromised optic nerve function. As discussed earlier, glaucoma occurs when the drainage of aqueous humor from the eye is impeded, leading to an elevation in IOP.
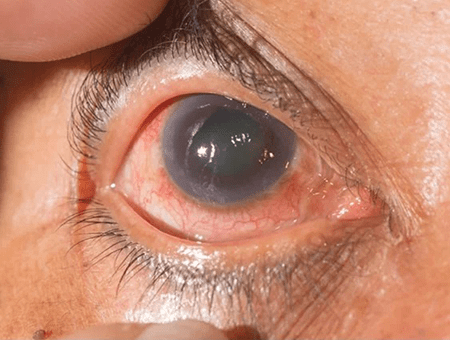
Various factors contribute to this obstruction, including anatomical abnormalities in the drainage angle, such as narrow angles or closed angles. Age-related changes in the eye’s structure and function can also contribute to the development of glaucoma.
Additionally, certain medical conditions, such as hypertension and diabetes, can affect the blood vessels in the eye, leading to impaired circulation and increased risk of glaucoma. Genetic predisposition and a family history of glaucoma further elevate the chances of developing the condition.
It is important to note that while increased IOP is a common risk factor, not all individuals with elevated IOP will develop glaucoma. Other factors, such as optic nerve health, blood flow, and individual susceptibility, play a role in determining the likelihood of glaucoma development.
In conclusion, glaucoma has various causes and risk factors, including elevated IOP, genetic predisposition, certain medical conditions, and anatomical abnormalities in the eye. Understanding these causes and risk factors is essential in early detection, prevention, and management of glaucoma. Regular eye examinations, especially for individuals at higher risk, are crucial for preserving vision and maintaining optimal eye health.
Glaucoma Causes

Glaucoma can arise from multiple factors, but the primary cause is an increase in intraocular pressure (IOP). The eye contains a clear fluid called aqueous humor, which is continuously produced and drained. When the drainage system becomes inefficient or blocked, the fluid accumulates, resulting in elevated IOP. This increased pressure inside the eye puts stress on the optic nerve, leading to damage over time.
Several risk factors can contribute to the development of glaucoma. Age is a significant factor, as the prevalence of glaucoma increases with advancing age. Family history of glaucoma also plays a role, indicating a genetic predisposition to the condition. People with a family history of glaucoma should be vigilant and undergo regular eye examinations to monitor their eye health.
Other risk factors include certain medical conditions, such as hypertension and diabetes, which can affect ocular blood flow and increase the risk of glaucoma. Additionally, individuals of African, Hispanic, or Asian descent have a higher susceptibility to glaucoma compared to other ethnic groups. Nearsightedness (myopia) and eye injuries may also contribute to the development of glaucoma.
Primary Open-Angle Glaucoma
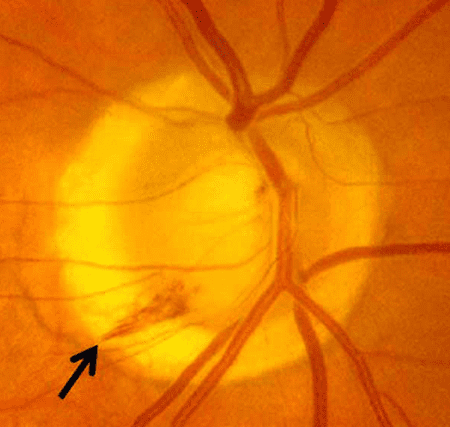
Primary open-angle glaucoma (POAG) is the most common form of glaucoma, accounting for around 90% of cases. The exact cause of POAG is not fully understood, but it is believed to result from a combination of genetic and environmental factors.
In POAG, the drainage angle of the eye remains open, but the drainage system becomes less efficient over time. This leads to a gradual buildup of fluid and an increase in IOP. As the pressure on the optic nerve persists, it can cause damage and gradually lead to vision loss.
While the specific causes of POAG are not entirely known, the risk factors mentioned earlier, such as family history and certain medical conditions, can contribute to its development. Regular eye check-ups and early detection are essential in managing POAG and preventing irreversible vision loss.
Angle-Closure Glaucoma

Angle-closure glaucoma, also known as closed-angle glaucoma or narrow-angle glaucoma, is less common than primary open-angle glaucoma. In angle-closure glaucoma, the drainage angle of the eye becomes blocked or obstructed, leading to a sudden increase in IOP.
This blockage may occur due to the iris being too close to the drainage angle or because the lens inside the eye pushes the iris forward, blocking the angle. When the angle is closed off, the aqueous humor cannot flow out of the eye, resulting in a rapid increase in IOP.
Angle-closure glaucoma can be classified as either acute or chronic. Acute angle-closure glaucoma is a medical emergency that requires immediate intervention to reduce IOP and prevent vision loss. Chronic angle-closure glaucoma, on the other hand, develops more gradually and may not exhibit severe symptoms initially.
Certain factors may trigger angle-closure glaucoma attacks, such as dim lighting, medications that dilate the pupils, or emotional stress. Individuals with a shallower anterior chamber depth, hypermetropia (farsightedness), or a family history of angle-closure glaucoma are at a higher risk. Timely diagnosis and appropriate treatment are crucial in managing angle-closure glaucoma effectively.
What is the most common glaucoma diagnosis (Ocular Hypertonia) ? :

The most common ocular hypertonia diagnosis is primary open-angle glaucoma (POAG). POAG is a chronic condition characterized by elevated intraocular pressure and progressive optic nerve damage. It is the most prevalent form of glaucoma and a leading cause of irreversible vision loss worldwide.
In POAG, the drainage angle of the eye appears normal, but there is a gradual decrease in the ability of the eye to drain fluid efficiently. This leads to an increase in intraocular pressure, which, if left untreated, can damage the optic nerve and result in vision loss.
While ocular hypertonia can exist independently without causing glaucoma, elevated intraocular pressure is a common feature of both conditions. Therefore, individuals with ocular hypertonia are at an increased risk of developing glaucoma, particularly primary open-angle glaucoma.
It is crucial for individuals diagnosed with ocular hypertonia, especially if it is associated with other risk factors such as family history or advanced age, to undergo regular monitoring and comprehensive eye examinations to detect any signs of glaucoma. Early diagnosis and appropriate management are essential in preserving vision and preventing the progression of glaucoma-related damage.
Ocular Hypertonia Diagnosis
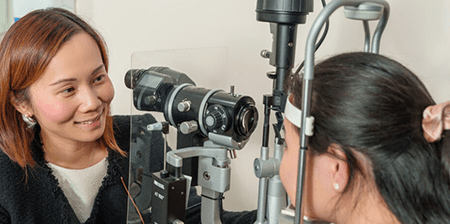
Diagnosing ocular hypertonia, or high intraocular pressure, involves a comprehensive evaluation of the eyes and their associated structures. The primary goal of the diagnostic process is to measure the intraocular pressure accurately and assess the overall health of the eye to determine the presence of ocular hypertonia.
One of the most common methods used to diagnose ocular hypertonia is tonometry. This procedure measures the pressure inside the eye by using various instruments, such as a tonometer or a non-contact tonometer. The intraocular pressure is typically expressed in millimeters of mercury (mmHg). Elevated intraocular pressure is a hallmark sign of ocular hypertonia, although it does not always indicate the presence of ocular hypertonia.
In addition to tonometry, a comprehensive eye examination is performed to evaluate other factors that may contribute to ocular hypertonia. This examination includes a thorough assessment of the optic nerve, visual field testing, and evaluation of the anterior segment of the eye. The optic nerve is carefully examined for any signs of damage or abnormalities. Visual field testing helps assess peripheral vision, which can be affected by ocular hypertonia. The examination of the anterior segment of the eye involves inspecting the drainage angle and evaluating the condition of the cornea and iris.
Ultimately, the diagnosis of ocular hypertonia requires a combination of clinical findings, including elevated intraocular pressure, optic nerve damage, visual field defects, and assessment of other relevant factors. It is important to note that the diagnosis of ocular hypertonia does not necessarily indicate the presence of ocular hypertonia, as the condition can exist independently without causing optic nerve damage or visual field loss.
Ocular Hypertonia Screening

Ocular hypertonia screening aims to detect early signs of ocular hypertonia, including ocular hypertonia, to initiate timely intervention and prevent vision loss. While routine eye examinations play a critical role in ocular hypertonia screening, specific tests and procedures may be performed to assess the risk and presence of ocular hypertonia.
One of the primary screening methods is tonometry, which measures intraocular pressure. Elevated intraocular pressure is a major risk factor for ocular hypertonia and prompts further evaluation. Another essential screening tool is the evaluation of the optic nerve through techniques like ophthalmoscopy or imaging tests such as optical coherence tomography (OCT). These assessments help identify any signs of optic nerve damage or structural abnormalities associated with ocular hypertonia.
Visual field testing is another crucial component of ocular hypertonia screening. This test examines the peripheral vision, which can be affected by ocular hypertonia. It helps identify any visual field defects that may indicate the presence of the disease.
Additionally, screening may involve assessing other risk factors such as family history, age, race, and certain medical conditions. Individuals with a family history of ocular hypertonia, advanced age (especially over 40 years), African descent, or certain systemic conditions such as diabetes are considered at higher risk and may require more frequent screening.
It is important to note that ocular hypertonia screening does not provide a definitive diagnosis but serves as an initial assessment to identify individuals who may require further evaluation and specialized care. A comprehensive eye examination by an eye care professional is necessary to confirm the diagnosis and determine the appropriate treatment plan.
Comprehensive Eye Exam

A comprehensive eye exam is an essential component of ocular hypertonia diagnosis and management. This comprehensive evaluation assesses not only the presence of ocular hypertonia but also other eye conditions or diseases that may contribute to vision loss.
During a comprehensive eye exam, the eye care professional will evaluate visual acuity, refractive error, and eye muscle movement. They will also assess the front structures of the eye, including the cornea, iris, and lens, to ensure their health and functionality.
Furthermore, the exam will include a dilated examination of the retina and optic nerve. This allows for a detailed assessment of the optic nerve head, nerve fiber layer, and blood vessels. Any abnormalities or signs of ocular hypertonia-related damage can be identified and monitored.
Comprehensive eye exams should be conducted regularly, especially for individuals at higher risk or those diagnosed with ocular hypertonia. Early detection and ongoing monitoring are crucial in managing glaucoma effectively and preserving vision.
What is the best treatment for glaucoma (Ocular Hypertonia)? :
The best treatment for ocular hypertonia depends on various factors, including the individual’s specific condition, response to treatment, and the extent of the disease. It is important to consult with an ophthalmologist or glaucoma specialist who can evaluate the condition and recommend the most appropriate treatment approach.
The treatment plan for ocular hypertonia often involves a combination of medication, laser trabeculoplasty, and, in some cases, surgical interventions. Medications are typically the first line of treatment, aiming to lower IOP and prevent further damage to the optic nerve. Laser trabeculoplasty may be considered when medications are insufficient or as an initial treatment option for certain cases. Surgical interventions are reserved for situations where other treatments have been unsuccessful or are deemed necessary based on the severity and progression of the condition.
Glaucoma (Ocular Hypertonia) Treatment
The primary goal of ocular hypertonia treatment is to reduce intraocular pressure (IOP) and prevent further damage to the optic nerve. Various treatment options are available, ranging from medication to surgical interventions.
-
Medication: Eyedrops are commonly prescribed as the first line of treatment for ocular hypertonia. These eyedrops work by either reducing the production of aqueous humor (the fluid in the eye) or increasing its drainage. Some examples of commonly prescribed eye drops include prostaglandin analogs, beta-blockers, alpha-adrenergic agonists, and carbonic anhydrase inhibitors. The specific medication and dosage depend on the individual’s condition and response to treatment.
-
Laser Trabeculoplasty: Laser trabeculoplasty is a surgical procedure used to lower intraocular pressure in individuals with ocular hypertonia. During the procedure, a laser is applied to the trabecular meshwork, which is responsible for draining the fluid from the eye. The laser energy helps improve the drainage of aqueous humor, reducing IOP. Laser trabeculoplasty is often considered when medications fail to adequately control IOP or as an initial treatment option for certain types of ocular hypertonia.
-
Surgical Interventions: In some cases, when medication and laser trabeculoplasty are ineffective or unsuitable, surgical interventions may be recommended. These procedures aim to create alternative pathways for fluid drainage or decrease the production of aqueous humor. Examples of surgical interventions for ocular hypertonia include trabeculectomy, drainage implants, and minimally invasive glaucoma surgeries (MIGS). These procedures are typically performed by ophthalmologists with expertise in glaucoma management.
Intraocular Pressure Management
Managing intraocular pressure is a key aspect of treating ocular hypertonia. Lowering IOP helps prevent optic nerve damage and slows down the progression of the condition. In addition to medication and surgical interventions, lifestyle modifications and regular monitoring play a crucial role in managing IOP.
-
Lifestyle Modifications: Certain lifestyle changes can help manage intraocular pressure. These may include maintaining a healthy weight, regular exercise, avoiding excessive eye rubbing, reducing caffeine intake, and managing stress levels. These lifestyle modifications may not replace the need for medication or surgery but can complement the overall treatment plan.
-
Regular Monitoring: Monitoring intraocular pressure is essential to assess the effectiveness of treatment and ensure its ongoing management. This involves regular visits to an ophthalmologist or eye care professional for comprehensive eye examinations and IOP measurements. It allows for early detection of changes in IOP and prompt adjustment of treatment if necessary.
What is the first line medication for glaucoma (Ocular Hypertonia)? :
The first-line medication for ocular hypertonia is typically a prostaglandin analog. These eye drops are highly effective in reducing intraocular pressure and are well-tolerated by most individuals. Due to their once-daily dosing convenience and sustained IOP-lowering effects, prostaglandin analogs are often recommended as the initial treatment option for individuals with ocular hypertonia.
However, the choice of medication may vary based on individual factors such as the severity of the condition, other medical conditions or allergies, and the patient’s response to treatment. In some cases, a combination of medications, including beta-blockers or other classes of glaucoma medications, may be prescribed to achieve optimal IOP control and manage ocular hypertonia effectively.
It is crucial to work closely with an ophthalmologist or eye care specialist to determine the most appropriate medication regimen for ocular hypertonia and ensure regular follow-up for monitoring and adjustments as needed. Early detection and effective management of ocular hypertonia play a vital role in preserving vision and preventing vision loss.
Ocular Hypertonia Medications:
Ocular hypertonia, characterized by elevated intraocular pressure (IOP), requires effective medication to reduce the pressure and prevent further damage to the optic nerve. Two commonly prescribed classes of medications for managing ocular hypertonia are prostaglandin analogs and beta-blockers. In this article, we will delve into the details of these medications and their role in controlling IOP.
Prostaglandin Analogs:
Prostaglandin analogs are a class of eye drops that are widely used as the first-line treatment for ocular hypertonia. These eye drops work by increasing the drainage of aqueous humor, the fluid inside the eye, thus lowering IOP. They are highly effective in reducing intraocular pressure and are often used as the initial treatment option due to their potency and once-daily dosing convenience.
One of the significant advantages of prostaglandin analogs is their ability to provide sustained IOP reduction over a 24-hour period. Commonly prescribed prostaglandin analogs include latanoprost, bimatoprost, travoprost, and tafluprost. These eye drops are well-tolerated by most individuals, and side effects are generally mild, including mild eye irritation, redness, or darkening of the iris or eyelashes.
Beta-Blockers:
Beta-blockers are another class of medications used to manage ocular hypertonia by reducing the production of aqueous humor. These eye drops work by blocking the beta-adrenergic receptors in the eye, which results in decreased fluid production and subsequently lowers intraocular pressure.
Beta-blockers are commonly prescribed either alone or in combination with other eye drops. They are known for their effectiveness in lowering IOP, and their efficacy can be further enhanced when used in combination with prostaglandin analogs. Commonly prescribed beta-blockers for ocular hypertonia include timolol, betaxolol, and levobunolol.
While beta-blockers are generally well-tolerated, individuals with respiratory conditions such as asthma or chronic obstructive pulmonary disease (COPD) may need to use them with caution due to potential systemic side effects. In such cases, alternative medications may be considered.
What surgery is done for glaucoma (Ocular Hypertonia)? :
The choice of surgery for ocular hypertonia depends on various factors, including the severity of the condition, individual patient characteristics, and the response to conservative treatments. Trabeculectomy and minimally invasive glaucoma surgery (MIGS) are two common surgical options.
Trabeculectomy is a well-established surgical procedure that creates a new drainage pathway to lower IOP. It is typically recommended for individuals with moderate to severe ocular hypertonia who have not achieved adequate IOP control with medications or other conservative treatments. Trabeculectomy can effectively lower IOP and preserve vision, but it is important to consider the potential risks and complications associated with this surgery.
MIGS procedures, on the other hand, are newer surgical techniques that aim to achieve IOP reduction with minimal invasiveness. They are often recommended for individuals with mild to moderate ocular hypertonia or as adjunct procedures during cataract surgery. MIGS procedures offer the advantages of shorter recovery times and reduced risks compared to traditional surgeries, but their suitability and effectiveness may vary depending on individual circumstances.
The choice of surgery for ocular hypertonia should be made in consultation with an ophthalmologist or glaucoma specialist who can assess the specific needs and circumstances of each patient. Regular follow-up visits and adherence to post-operative care instructions are essential for monitoring the success of the surgery and managing any potential complications.
Surgical Options for Ocular Hypertonia:
When medications and other conservative treatments are unable to effectively manage ocular hypertonia, surgical intervention may be necessary. Surgical procedures aim to lower intraocular pressure (IOP) and prevent further damage to the optic nerve. Two commonly performed surgeries for ocular hypertonia are trabeculectomy and minimally invasive glaucoma surgery (MIGS). In this article, we will delve into the details of these surgical options and their role in treating ocular hypertonia.
Trabeculectomy:
Trabeculectomy is a conventional surgical procedure used for reducing IOP in individuals with ocular hypertonia. During this surgery, a small opening is created in the sclera (white part of the eye) to allow the drainage of aqueous humor, the fluid inside the eye. This helps to lower IOP and prevent damage to the optic nerve.
Trabeculectomy is typically performed under local anesthesia and involves the use of sutures to create a filtering bleb, which is a small reservoir under the conjunctiva (thin, clear tissue covering the white part of the eye). The bleb allows excess aqueous humor to drain out, reducing the pressure within the eye.
While trabeculectomy has a high success rate in lowering IOP, it is considered an invasive procedure and may be associated with certain risks and complications. These can include infection, bleeding, scarring, and cataract formation. Regular post-operative follow-up visits with an ophthalmologist are crucial to monitor the success of the surgery and manage any potential complications.
Minimally Invasive Glaucoma Surgery (MIGS):
Minimally invasive glaucoma surgery (MIGS) represents a newer approach to surgical intervention for ocular hypertonia. Unlike traditional glaucoma surgeries, MIGS procedures are designed to be less invasive, with the goal of reducing IOP while minimizing the risks and complications associated with more invasive surgeries.
MIGS procedures involve the use of specialized devices and techniques to improve the drainage of aqueous humor and lower IOP. These procedures are typically performed in conjunction with cataract surgery or as standalone procedures. Some common MIGS procedures include the implantation of microstents, trabecular meshwork bypass, and suprachoroidal shunts.
The advantages of MIGS procedures include shorter surgical times, faster recovery, and reduced post-operative complications compared to more invasive surgeries. However, it is important to note that MIGS may not be suitable for all individuals with ocular hypertonia, and the selection of the most appropriate surgical approach should be based on individual factors and the recommendations of an ophthalmologist.
How can I prevent glaucoma at home (Ocular Hypertonia)? :
While you cannot entirely prevent ocular hypertonia at home, there are steps you can take to promote overall eye health and potentially reduce the risk of developing this condition. These include:
-
Regular Eye Exams: Schedule routine eye examinations with an ophthalmologist or optometrist to monitor your eye health, especially if you have a family history of ocular hypertonia. Early detection and intervention can help manage the condition more effectively.
-
Maintain a Healthy Lifestyle: Adopt a balanced diet rich in eye-healthy nutrients, engage in regular exercise, avoid smoking, and moderate alcohol consumption. These lifestyle choices contribute to overall eye health and may help reduce the risk of ocular hypertonia.
-
Protect Your Eyes: Wear appropriate eye protection, such as safety glasses or goggles, during activities that pose a risk of eye injury. Shielding your eyes from potential trauma can help prevent damage that may contribute to ocular hypertonia.
-
Manage Systemic Health: Control underlying health conditions, such as diabetes or hypertension, through regular medical care and adherence to prescribed treatments. Managing systemic health conditions can have a positive impact on overall eye health.
It is important to remember that while these measures can contribute to maintaining healthy eyes and potentially reducing the risk of ocular hypertonia, regular professional eye care and monitoring remain crucial for early detection and appropriate management of any eye condition.
Preventing Ocular Hypertonia:
While ocular hypertonia cannot be completely prevented, certain measures can be taken to reduce the risk of developing this condition or to manage its progression. Prevention strategies primarily focus on maintaining a healthy lifestyle and being aware of family history. By incorporating these practices into your daily routine, you can potentially lower the risk of ocular hypertonia and minimize its impact on your eye health.
Healthy Lifestyle:
Adopting a healthy lifestyle can play a significant role in reducing the risk of ocular hypertonia. Regular exercise, such as brisk walking or jogging, helps improve blood circulation throughout the body, including the eyes. Engaging in physical activity also promotes overall cardiovascular health, which can indirectly benefit the eyes by maintaining optimal blood flow.
Additionally, maintaining a balanced diet rich in fruits, vegetables, and omega-3 fatty acids has been associated with a lower risk of developing certain eye conditions, including ocular hypertonia. These nutrients provide essential antioxidants and anti-inflammatory properties that can support eye health.
Avoiding smoking and excessive alcohol consumption is also important. Smoking has been linked to an increased risk of developing glaucoma and worsening its progression. Similarly, excessive alcohol consumption can raise intraocular pressure, leading to ocular hypertonia.
Family History of Ocular Hypertonia:
Family history plays a significant role in the development of ocular hypertonia. If you have a family member with ocular hypertonia or glaucoma, it is important to be aware of your increased risk and take proactive measures to monitor your eye health.
Regular eye examinations are crucial, as they can help detect early signs of ocular hypertonia or other eye conditions. Your eye care professional can measure your intraocular pressure and assess the health of your optic nerve to identify any abnormalities.
Knowing your family history also allows you to inform your eye care provider, enabling them to tailor your eye exams and screenings accordingly. They may recommend more frequent check-ups or additional diagnostic tests to closely monitor your eye health.
What naturally helps glaucoma (Ocular Hypertonia)? :
While yoga and acupuncture are among the natural remedies that may provide some relief for ocular hypertonia, it is important to note that they should be used as complementary approaches alongside conventional medical treatment. They should not replace professional medical advice or prescribed treatments.
In addition to yoga and acupuncture, several lifestyle factors may help support eye health and potentially alleviate ocular hypertonia symptoms:
-
Balanced Diet: Consuming a diet rich in antioxidants, vitamins, and minerals can promote overall eye health. Include foods such as leafy green vegetables, fruits, nuts, and fish in your diet.
-
Stress Reduction: Managing stress through techniques like meditation, deep breathing exercises, and mindfulness practices can help promote relaxation and potentially reduce intraocular pressure.
-
Regular Exercise: Engaging in regular physical activity can support cardiovascular health, improve blood circulation, and contribute to overall well-being, which may indirectly benefit eye health.
-
Adequate Hydration: Staying hydrated by drinking plenty of water can help maintain overall health and proper eye function.
It is essential to consult with your healthcare provider or ophthalmologist before incorporating any natural remedies or complementary therapies into your treatment plan. They can provide guidance based on your individual condition and help ensure the safety and efficacy of these approaches.
Natural Remedies for Ocular Hypertonia:
While there is no cure for ocular hypertonia, some natural remedies and complementary therapies may help in managing the condition and promoting overall eye health. Two such approaches are yoga and acupuncture, which have gained attention for their potential benefits in supporting eye health and reducing intraocular pressure.
Yoga for Ocular Hypertonia:
Yoga is a holistic practice that combines physical postures, breathing exercises, and meditation. It has been found to offer various health benefits, including stress reduction, improved circulation, and relaxation. Certain yoga poses and techniques specifically target eye health and may be beneficial for individuals with ocular hypertonia.
One commonly recommended yoga exercise for eye health is palming. It involves covering the eyes with cupped hands while gently placing the palms over the eyes, allowing the eyes to rest and relax. Palming helps reduce eye strain and promote relaxation of the eye muscles, potentially alleviating some of the pressure associated with ocular hypertonia.
Other yoga poses that promote blood circulation and relaxation, such as forward bends, shoulder stands, and inversions, may indirectly benefit eye health by reducing stress and enhancing overall well-being.
Acupuncture for Ocular Hypertonia:
Acupuncture is a traditional Chinese medicine technique that involves the insertion of thin needles into specific points on the body. It is believed to stimulate energy flow and promote balance within the body. Acupuncture has been explored as a potential complementary therapy for ocular hypertonia.
Acupuncture treatments for ocular hypertonia typically target specific acupuncture points related to eye health and overall well-being. The stimulation of these points is thought to help regulate intraocular pressure and improve blood circulation to the eyes.
Although some studies suggest that acupuncture may have a positive impact on intraocular pressure, the evidence is limited, and further research is needed to establish its efficacy as a standalone treatment for ocular hypertonia. It is important to consult with a qualified acupuncture practitioner and inform your eye care professional if you are considering acupuncture as a complementary therapy.
Related Links
Conclusion:
In conclusion, ocular hypertonia, or high intraocular pressure, is a condition that requires proper management to prevent vision loss and maintain eye health. While there is no known cure for ocular hypertonia, various treatment options are available to control intraocular pressure and minimize the risk of complications. These include medications, surgical procedures, and lifestyle modifications. It is essential for individuals with ocular hypertonia to work closely with their healthcare providers or ophthalmologists to develop a personalized treatment plan that suits their specific needs.
Furthermore, prevention plays a crucial role in managing ocular hypertonia. Regular eye examinations, especially for individuals with a family history of the condition, can help detect early signs and enable timely intervention. Adopting a healthy lifestyle, including a balanced diet, regular exercise, stress management, and adequate hydration, can contribute to overall eye health and potentially reduce the risk of ocular hypertonia.
While natural remedies and complementary therapies such as yoga and acupuncture may offer certain benefits for ocular hypertonia, they should be used in conjunction with conventional medical treatments. It is important to consult with healthcare professionals before incorporating any new approaches into the treatment plan.
By raising awareness about ocular hypertonia, its causes, symptoms, diagnosis, treatment options, and preventive measures, individuals can take proactive steps to preserve their eye health and minimize the impact of this condition on their vision.
Q: 1. Can ocular hypertonia be cured?
A: Ocular hypertonia, or high intraocular pressure, is a chronic condition that currently has no cure. However, with appropriate management, including medications, surgical interventions, and lifestyle modifications, it is possible to control intraocular pressure and prevent vision loss.
Q: 2. Are there any natural remedies for ocular hypertonia?
A: While there are natural remedies and complementary therapies such as yoga and acupuncture that may provide certain benefits for ocular hypertonia, they should be used as adjunctive approaches alongside conventional medical treatments. It is crucial to consult with healthcare professionals before incorporating any natural remedies into the treatment plan.
Q: 3. How often should I have my eyes checked for ocular hypertonia?
A: Regular eye examinations are essential for individuals with ocular hypertonia, especially those with a family history of the condition. The frequency of eye check-ups may vary depending on individual circumstances, but it is generally recommended to have comprehensive eye exams every 1-2 years or as advised by your eye care professional.
Q: 4. Can lifestyle changes help in managing ocular hypertonia?
A: Yes, adopting a healthy lifestyle can contribute to the management of ocular hypertonia. Maintaining a balanced diet, engaging in regular exercise, managing stress, and staying adequately hydrated can support overall eye health and potentially reduce the risk of complications associated with ocular hypertonia.
Q: 5. Is ocular hypertonia a reversible condition?
A: While ocular hypertonia itself may not be reversible, its progression and associated complications can be managed through proper treatment and ongoing care. By controlling intraocular pressure and implementing preventive measures, individuals with ocular hypertonia can help maintain their eye health and minimize the impact on their vision.
More Links
What is ocular hypertonia? |
Group of ocular hypertonia |
Symptoms of ocular hypertonia. |
Open-angle ocular hypertonia |