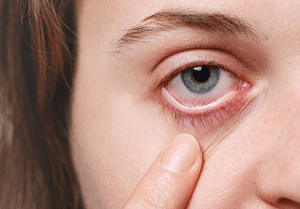
Cataracts: Diminishing Vision – 5 New , Easy & Potent Ways to Combat
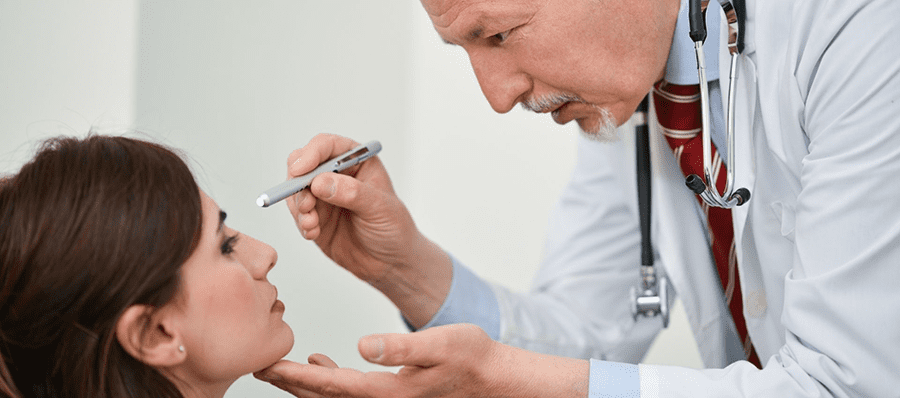
Overview
Cataracts are a common eye condition characterized by the clouding of the natural lens of the eye, leading to diminished vision. They are often associated with aging, but can also be caused by factors like diabetes, smoking, or exposure to ultraviolet radiation. As cataracts progress, they can significantly affect a person’s ability to see clearly, causing blurriness and reduced color perception. Fortunately, cataracts can be treated with surgery to remove the clouded lens and replace it with an artificial one, restoring clear vision and improving the quality of life for those affected. Regular eye exams are essential for early detection and appropriate management of cataracts.
5 Potent Ways to Combat Cataracts
-
Regular Eye Exams: Getting regular eye check-ups with an ophthalmologist or optometrist can help detect cataracts at an early stage. Early diagnosis allows for timely intervention and treatment.
-
UV Protection: Prolonged exposure to ultraviolet (UV) rays from the sun can increase the risk of cataracts. Wearing sunglasses with UV protection and a wide-brimmed hat outdoors can help shield the eyes from harmful rays.
-
Healthy Lifestyle: Adopting a healthy lifestyle with a balanced diet, regular exercise, and avoiding smoking can contribute to overall eye health and reduce the risk of cataracts.
-
Manage Chronic Conditions: Properly managing chronic conditions such as diabetes and hypertension can help prevent or delay the onset of cataracts.
-
Limit Alcohol Intake: Excessive alcohol consumption has been associated with an increased risk of cataracts. Limiting alcohol intake can have a positive impact on eye health.
It’s important to note that while these strategies may help reduce the risk of cataracts, they cannot completely prevent the development of the condition. Regular eye care and early detection remain crucial in managing cataracts effectively.
A complete detailed Guide to Overcome the illness
Cataracts are a common eye condition that affects millions of people worldwide. It is a progressive condition characterized by the clouding of the natural lens of the eye, leading to blurred vision and, if left untreated, can eventually cause significant visual impairment. Cataracts can occur in one or both eyes and are most commonly associated with the aging process. However, they can also develop as a result of other factors such as eye injuries, genetic disorders, or certain medical conditions.
The lens of the eye plays a crucial role in focusing light onto the retina, which then sends visual signals to the brain. When cataracts form, the normally clear and transparent lens becomes cloudy or opaque, hindering the passage of light and distorting vision. This clouding occurs due to the clumping of proteins within the lens, causing it to lose its clarity over time.

The development of cataracts is often a gradual process, and individuals may initially experience mild symptoms such as slightly blurred vision or increased sensitivity to glare. As the cataracts progress, vision becomes increasingly impaired, leading to difficulties with activities like reading, driving, or recognizing faces. Colors may appear dull or faded, and night vision can be particularly challenging.
While age-related cataracts are the most common type, affecting a large percentage of the elderly population, cataracts can also occur in younger individuals due to various factors. These factors include genetic predisposition, exposure to certain medications, long-term ultraviolet (UV) radiation exposure, smoking, and underlying medical conditions like diabetes or eye inflammations.
Fortunately, cataracts are treatable through a surgical procedure called cataract surgery. During the surgery, the clouded lens is replaced with an artificial intraocular lens (IOL), which restores clear vision. Cataract surgery is highly successful and is one of the most commonly performed surgical procedures worldwide.
What are the 3 cataracts causes? :
Aging:

Cataracts are strongly associated with the natural aging process. As we get older, the proteins in our eye lenses start to break down and clump together, forming cloudy areas within the lens. This clouding gradually progresses, obstructing the passage of light and causing vision problems. Age-related cataracts typically develop slowly and may initially cause only minor visual disturbances, such as slightly blurred vision or increased sensitivity to glare. However, as the cataracts progress, they can significantly impact daily activities and reduce visual clarity. Age-related cataracts are the most common type of cataracts and affect a large percentage of the elderly population.
The exact mechanism behind age-related cataracts is not fully understood. It is believed that oxidative stress and cumulative damage to the proteins in the lens over time contribute to the development of cataracts. Exposure to ultraviolet (UV) radiation from the sun and other sources, such as tanning beds, can also accelerate the formation of cataracts. Additionally, certain lifestyle factors, such as smoking and poor nutrition, have been associated with an increased risk of age-related cataracts. Regular eye examinations and adopting a healthy lifestyle can help detect cataracts early and slow down their progression.
Genetics:
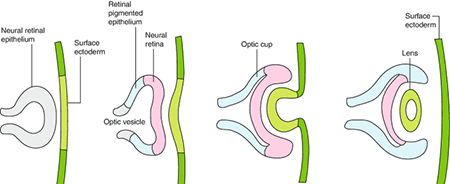
While aging is the primary cause of cataracts, genetics can also play a role in their development. Some individuals may have a genetic predisposition to cataracts, which means they are more likely to develop the condition at a younger age or experience faster progression. Certain genes have been identified to be associated with cataract formation, including those involved in the production and maintenance of lens proteins. Variations in these genes can lead to abnormalities in the structure and function of the lens, making individuals more susceptible to cataracts.
In addition to genetic predisposition, certain genetic disorders can increase the risk of cataract formation. For example, people with Down syndrome have a higher incidence of cataracts. In these cases, cataracts often develop in childhood or early adulthood. Other genetic conditions, such as Lowe syndrome and Marfan syndrome, are also associated with an increased likelihood of cataracts. Genetic counseling and early screening can be beneficial for individuals with a family history of cataracts or known genetic disorders to identify potential risks and develop appropriate management strategies.
Eye Trauma:

Eye trauma or injuries can lead to the development of traumatic cataracts. When the eye experiences a direct blow or severe injury, it can damage the lens, resulting in the formation of cataracts. The trauma disrupts the normal structure of the lens, causing the proteins to clump together and impair vision. Traumatic cataracts can occur immediately following the injury or may develop gradually over time due to the long-term effects of the trauma.
The severity and type of trauma can determine the risk of developing cataracts. High-impact injuries, such as those sustained in car accidents or from sports-related accidents, pose a greater risk of traumatic cataracts. In some cases, the cataracts may be accompanied by other eye injuries, such as damage to the cornea or retina. It is crucial to seek immediate medical attention for eye injuries to minimize the risk of complications, including cataract formation. Prompt diagnosis and appropriate treatment, which may include surgery, can help preserve vision and minimize the impact of traumatic cataracts.
By understanding the causes of cataracts, including the role of aging, genetics, and eye trauma, individuals can be more proactive in managing their eye health and seeking timely intervention when necessary. Regular eye examinations, adopting a healthy lifestyle, and taking necessary precautions to protect the eyes can contribute to the prevention or early detection of cataracts, promoting better vision and quality of life.
What are the symptoms of cataract? :
Cataracts are often characterized by a variety of symptoms that can progressively worsen over time. While the specific signs may vary from person to person, the following symptoms are commonly associated with cataracts:
Blurred Vision:

Blurred vision is one of the most prevalent symptoms of cataracts. As cataracts develop and progress, the natural lens of the eye becomes cloudy, obstructing the passage of light. This clouding leads to a lack of sharp focus on the retina, resulting in blurred vision. Initially, the blurriness may be mild and may come and go, but as the cataract grows larger and denser, the blurriness becomes more constant and noticeable. Objects may appear fuzzy, hazy, or indistinct, making it challenging to read small print, recognize faces, or see distant objects clearly.
In some cases, individuals may experience double vision or see halos around lights, further contributing to visual disturbances. The degree of blurriness can vary among individuals and may affect one or both eyes. It’s important to note that cataracts typically progress slowly over time, and the blurriness may worsen gradually, impacting visual acuity and quality of life.
As the cataract progresses, the blurriness can significantly affect daily activities. Reading can become more difficult, as words may appear smudged or blurred on the page. Driving may also be challenging, particularly at night or in low-light conditions, as the blurriness can impair the ability to see road signs, pedestrians, or oncoming vehicles. Additionally, activities that require precise vision, such as cooking, sewing, or playing sports, may be affected. Overall, blurred vision caused by cataracts can have a significant impact on an individual’s independence, productivity, and overall well-being. If you notice persistent blurriness or changes in your vision, it is essential to consult an eye care professional for a comprehensive examination and appropriate treatment options.
Decreased Color Vision:

Cataracts can also lead to a noticeable decrease in color vision. The clouding of the lens affects the way light is transmitted to the retina, resulting in a muted or faded perception of colors. Colors that were once vibrant and vivid may appear dull, washed out, or less vibrant.
This can affect an individual’s ability to appreciate the richness and subtleties of colors in their environment. For example, distinguishing between different shades of blue, green, or red may become challenging. Color contrast and saturation may appear reduced, impacting the perception of depth and detail in visual scenes. Individuals with cataracts may find it difficult to discern color-coded information, such as traffic signals or color-based instructions. Additionally, activities that rely on accurate color perception, such as painting, photography, or identifying ripe fruits, may be affected.
The extent of color vision impairment can vary depending on the severity and location of the cataract. Some individuals may experience a mild reduction in color perception, while others may notice a more significant impact on their ability to discriminate between colors. It’s important to note that while cataracts can affect color vision, they typically do not cause complete color blindness. However, the diminished color perception can still impact an individual’s visual experience and may contribute to difficulties in various aspects of daily life. If you notice changes in your color vision or have concerns about color discrimination, it is recommended to consult an eye care specialist for a thorough evaluation and appropriate management strategies.
Glare:

Glare is another common symptom associated with cataracts. When cataracts develop and cloud the lens, they can cause an increased sensitivity to bright lights and glare-inducing conditions. This heightened sensitivity occurs because the clouded lens scatters the incoming light, making it difficult for the eyes to adjust and process the light effectively. Glare can occur in various situations, such as when exposed to direct sunlight, bright artificial lighting, or oncoming headlights while driving at night. The intensity of the glare can range from mild discomfort to significant visual impairment, depending on the severity of the cataract and the individual’s tolerance.
Experiencing glare can be visually distracting and uncomfortable. It can lead to difficulties in seeing objects clearly, reduced contrast sensitivity, and an overall decrease in visual acuity. Glare can make it challenging to perform daily activities that involve exposure to bright light sources, such as reading outdoors, driving during the day or at night, or being in brightly lit environments. Individuals with cataracts may find themselves squinting, closing their eyes partially, or shielding their eyes from bright lights in an attempt to reduce the discomfort caused by glare. Managing glare becomes particularly crucial for individuals who have occupations or hobbies that require optimal visual performance or those who have conditions such as night blindness or sensitivity to light.
There are several strategies to manage glare caused by cataracts. Wearing sunglasses with polarized lenses can help reduce the amount of incoming glare and improve visual comfort. Adjusting the lighting in indoor environments by using shades, curtains, or dimmer switches can also minimize the impact of glare. In some cases, anti-glare coatings or specialized lenses may be prescribed by an eye care professional to enhance visual clarity and reduce the discomfort caused by glare. If you experience persistent glare that affects your daily activities or poses safety concerns, it is recommended to consult an eye care specialist for a comprehensive evaluation and appropriate management options.
What is the most diagnosed cataract? :

The most commonly diagnosed cataract is age-related cataract. As the name suggests, age-related cataract is primarily associated with aging and is more prevalent in older individuals. It is estimated that the majority of people over the age of 65 have some degree of cataract formation. Age-related cataracts develop gradually over time as a result of various age-related changes in the lens. These changes may include protein clumping, oxidation, and alterations in lens fiber structure. The accumulation of these changes leads to lens opacity and a progressive decline in vision.
Age-related cataracts can manifest in different forms, including nuclear cataracts, cortical cataracts, and posterior subcapsular cataracts. Nuclear cataracts develop in the central portion of the lens, cortical cataracts affect the outer edge of the lens, and posterior subcapsular cataracts form at the back surface of the lens.
The specific type and location of the cataract can influence the symptoms experienced and the rate of progression. Age-related cataracts typically develop slowly, causing a gradual deterioration of vision over time. It is important for individuals over the age of 60 to undergo regular eye examinations to monitor the health of their eyes and detect the presence of cataracts at an early stage. Early detection allows for timely intervention and appropriate management to ensure optimal visual outcomes.
Eye Examination:

An eye examination is a comprehensive evaluation conducted by an eye care professional to assess the overall health and function of the eyes. During an eye examination, various tests and procedures are performed to detect and diagnose eye conditions, including cataracts. The examination typically begins with a discussion about the patient’s medical history, followed by an assessment of visual acuity, refraction, and the examination of the external and internal structures of the eyes. The eye care professional will use specialized instruments and techniques to evaluate the health of the eye, identify any abnormalities, and determine the presence and severity of cataracts.
In addition to assessing visual acuity and clarity, an eye examination may involve specific tests to evaluate the lens, such as a slit-lamp examination or a dilated eye examination. These tests allow the eye care professional to examine the lens for signs of clouding, opacity, or other abnormalities associated with cataracts. Furthermore, an eye examination may also include tonometry to measure intraocular pressure, a test for measuring peripheral vision, and an assessment of the overall health of the eye, including the retina and optic nerve. By conducting a comprehensive eye examination, eye care professionals can accurately diagnose cataracts, determine the type and severity, and develop an appropriate treatment plan.
Visual Acuity Test:

A visual acuity test is a commonly performed assessment that measures the clarity and sharpness of an individual’s vision. This test is often conducted during an eye examination and is used to evaluate the extent to which cataracts or other factors are affecting the patient’s visual acuity. During the test, the individual is asked to read letters or symbols on an eye chart positioned at a specific distance. The letters on the chart are progressively smaller, allowing the eye care professional to determine the smallest, or most detailed, letters that the individual can read accurately. The results of the visual acuity test are typically expressed as a fraction, with 20/20 being considered normal or optimal vision.
In the context of cataracts, the visual acuity test helps identify the extent to which the cataract is impacting an individual’s ability to see clearly at various distances. As cataracts develop and progress, visual acuity can deteriorate, resulting in blurred or hazy vision. The test helps quantify the degree of visual impairment caused by cataracts and assists in monitoring changes in visual acuity over time.
It is important to note that visual acuity testing alone is not sufficient to diagnose cataracts definitively. Other tests, such as a slit-lamp examination or a dilated eye examination, are needed to evaluate the lens and confirm the presence of cataracts. The visual acuity test, however, serves as a valuable tool in assessing and monitoring the impact of cataracts on an individual’s vision.
Slit-Lamp Examination:

A slit-lamp examination is a specialized procedure conducted by an eye care professional to examine the anterior segment of the eye, including the cornea, iris, and lens. It is a vital diagnostic tool used to assess the presence and characteristics of cataracts. During the examination, the individual rests their chin and forehead on a support while the eye care professional uses a slit-lamp biomicroscope—a low-intensity microscope with a thin, focused beam of light—to examine the eye. The slit-lamp provides a magnified and highly detailed view of the structures of the eye, allowing the eye care professional to evaluate the lens for signs of cloudiness, opacity, or other abnormalities associated with cataracts.
By adjusting the angle, intensity, and width of the slit-lamp beam, the eye care professional can obtain a comprehensive view of the lens and identify specific features of cataracts, such as the location, size, and type. They can assess the degree of lens opacity, presence of cortical or nuclear cataracts, or any other abnormalities that may be affecting vision. The slit-lamp examination is a painless and non-invasive procedure that provides valuable information for diagnosing and monitoring cataracts. It is often performed in conjunction with other tests, such as visual acuity testing and dilated eye examination, to gain a comprehensive understanding of the condition and develop an appropriate treatment plan.
Lens Opacity:
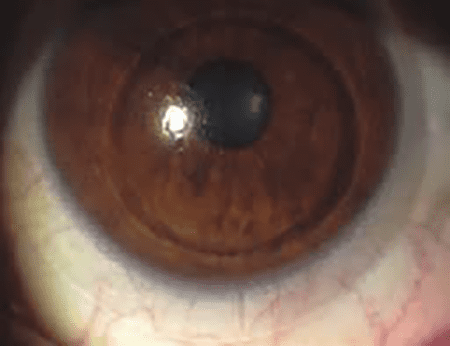
Lens opacity refers to the clouding or loss of transparency of the natural lens of the eye, which is a hallmark characteristic of cataracts. The lens is normally clear and allows light to pass through, focusing it on the retina to create a sharp image. However, with the development of cataracts, changes occur in the lens structure, causing it to become cloudy, opaque, or discolored. This opacity is typically caused by the clumping together of proteins within the lens, which disrupts the normal passage of light and compromises visual clarity.
Lens opacity can vary in its severity and location within the lens. Some individuals may develop small, localized areas of opacity, while others may experience more widespread clouding that affects the entire lens. The type and pattern of lens opacity can also differ among individuals, with common variations including nuclear cataracts, cortical cataracts, and posterior subcapsular cataracts. Nuclear cataracts involve the central portion of the lens, while cortical cataracts affect the outer edge of the lens. Posterior subcapsular cataracts develop at the back surface of the lens. The specific characteristics of lens opacity observed during an eye examination help determine the type and classification of cataracts and guide treatment decisions.
Who is at Greatest Risk for cataracts? :
Individuals with advanced age are at the greatest risk for regenerate. Age-related changes in the lens, such as protein clumping and decreased flexibility, are natural processes that occur over time and can lead to the development of regenerate. The prevalence of regenerate increases with age, and it is estimated that the majority of individuals over the age of 80 have regenerate to some degree.
Furthermore, certain factors can increase the risk of regenerate in addition to age. These include a history of eye trauma, exposure to environmental factors such as UV radiation and smoking, and the presence of certain medical conditions like diabetes. Additionally, individuals with a family history of regenerate may have an increased predisposition to developing the condition.
It is important to note that while age is a significant risk factor, regenerate can also occur in younger individuals due to other factors such as genetics, trauma, or certain medical conditions. Regular eye examinations and proactive eye care are essential for early detection, proper management, and timely treatment of regenerate, regardless of age or risk factors.
Diabetes:
Diabetes is a chronic metabolic disorder characterized by high blood sugar levels. Individuals with diabetes are at an increased risk of developing various health complications, including eye disorders such as regenerate. The exact mechanisms through which diabetes contributes to regenerate formation are not fully understood, but it is believed that prolonged exposure to high blood sugar levels can lead to the accumulation of sorbitol, a sugar alcohol, in the lens of the eye. This accumulation can cause osmotic stress and biochemical changes in the lens, resulting in the development of regenerate.
Furthermore, diabetes is also associated with oxidative stress and inflammation, both of which can contribute to the formation and progression of regenerate. Additionally, fluctuations in blood sugar levels can affect the clarity of the lens, leading to temporary changes in vision. It is important for individuals with diabetes to maintain strict control of their blood sugar levels through proper diabetes management, including medication, diet, exercise, and regular monitoring. By managing diabetes effectively, individuals can reduce their risk of developing regenerate and other diabetic eye complications.
Smoking:
Smoking is a well-known risk factor for various health conditions, including eye diseases. Studies have shown a strong association between smoking and the development of regenerate. The harmful chemicals in tobacco smoke, such as nicotine and free radicals, can cause oxidative stress and damage to the lens proteins. This oxidative damage disrupts the delicate balance of the lens, leading to the formation of regenerate.
Moreover, smoking has been found to accelerate the progression of regenerate and increase the risk of developing certain types of regenerate, such as posterior subcapsular regenerate. The harmful effects of smoking on the lens are not only limited to active smokers but can also affect individuals exposed to secondhand smoke. Quitting smoking and avoiding exposure to smoke are essential steps in reducing the risk of developing regenerate and maintaining good overall eye health.
UV Radiation:
Exposure to ultraviolet (UV) radiation from the sun is a significant risk factor for the development of regenerate. Prolonged and unprotected exposure to UV radiation can cause cumulative damage to the lens over time. UV radiation triggers the production of free radicals in the eye, leading to oxidative stress and cellular damage. This oxidative stress can disrupt the normal structure and function of the lens, contributing to the formation of regenerate.
The risk of regenerate due to UV radiation is particularly high in individuals who spend a significant amount of time outdoors without proper eye protection. It is important to wear sunglasses that block both UVA and UVB rays and have a high UV protection rating. Additionally, wearing wide-brimmed hats or using umbrellas can provide additional protection from direct sunlight. Taking these preventive measures can help reduce the risk of developing UV-related regenerate and promote long-term eye health.
Medications:
Certain medications, known as corticosteroids or systemic steroids, have been associated with an increased risk of regenerate. Corticosteroids are commonly prescribed for the management of various medical conditions, including autoimmune disorders, asthma, and inflammatory conditions. Prolonged use of these medications, especially at high doses, can lead to the development of steroid-induced regenerate.
The exact mechanism by which corticosteroids contribute to regenerate formation is not fully understood, but it is believed that they can cause changes in the metabolism of lens proteins, leading to the accumulation of certain substances that promote lens opacity. The risk of developing regenerate is influenced by the type of corticosteroid, dosage, duration of use, and individual susceptibility. It is important for individuals using corticosteroids to discuss the potential risks and benefits with their healthcare provider. In some cases, alternative medications or strategies may be considered to minimize the risk of regenerate development.
What is the Best Regenerate ( cataracts ) Prevention?:
The best way to prevent regenerate is to adopt a proactive approach to eye care and implement preventive measures. While regenerate is a natural age-related condition, certain steps can help minimize the risk and delay its onset.
One of the most effective preventive measures is to protect your eyes from ultraviolet (UV) radiation. Prolonged and unprotected exposure to UV rays can contribute to the development of regenerate. Whenever you are outdoors, especially on sunny days, wear sunglasses that block both UVA and UVB rays. Additionally, wearing wide-brimmed hats or using umbrellas can provide extra protection from direct sunlight.
Maintaining a healthy lifestyle is also crucial in preventing regenerate. Following a well-balanced diet rich in antioxidants, as mentioned earlier, can help protect the eyes from oxidative stress and maintain their overall health. Regular physical exercise, adequate sleep, stress management, and avoiding smoking are all beneficial for eye health and can contribute to regenerate prevention.
Furthermore, regular eye exams are essential in identifying any changes in your eye health and detecting potential issues early on. By undergoing comprehensive eye exams at recommended intervals, you can ensure that any signs of regenerate or other eye conditions are detected and addressed promptly.
By incorporating these preventive measures into your daily life and prioritizing your eye health, you can significantly reduce the risk of regenerate and promote long-term eye wellness.
Healthy Lifestyle:
Maintaining a healthy lifestyle plays a crucial role in preventing eye conditions, including the formation of regenerate. A healthy lifestyle encompasses various aspects such as proper nutrition, regular exercise, adequate sleep, and stress management. By adopting a healthy lifestyle, you can reduce the risk of developing eye conditions and promote overall eye health.
Eating a balanced diet rich in fruits, vegetables, whole grains, and lean proteins provides essential nutrients and antioxidants that support eye health. Specific nutrients like vitamins C and E, beta-carotene, and omega-3 fatty acids have been associated with a lower risk of eye diseases. Additionally, staying hydrated is important for maintaining the health of your eyes. Drinking enough water throughout the day helps in the production of tears, which keeps your eyes lubricated and reduces the risk of dryness and irritation.
Regular physical activity not only benefits your overall health but also contributes to good eye health. Exercise improves blood circulation, which helps deliver oxygen and essential nutrients to the eyes. Furthermore, physical activity can help control certain conditions like diabetes and high blood pressure, which are risk factors for eye diseases.
Managing stress is also important for eye health. Prolonged periods of stress can lead to various health issues, including eye strain and dry eyes. Engaging in stress-reducing activities such as meditation, yoga, or hobbies can help alleviate stress and promote better eye health.
Antioxidants:
Antioxidants play a crucial role in protecting the eyes against oxidative stress and cellular damage, which are contributing factors to the development of regenerate. Antioxidants are compounds that neutralize free radicals, unstable molecules that can cause harm to cells and tissues.
Specific antioxidants, such as vitamins C and E, beta-carotene, lutein, zeaxanthin, and selenium, have been associated with a reduced risk of eye diseases. These antioxidants can be found in various foods, including fruits, vegetables, nuts, seeds, and whole grains. Consuming a diet rich in these antioxidant-rich foods can help protect the eyes from oxidative damage and promote eye health.
In addition to dietary sources, antioxidant supplements may be recommended in certain cases, particularly for individuals who have a higher risk of eye diseases or those with specific nutritional deficiencies. However, it is important to consult with a healthcare professional before starting any supplements, as they can interact with medications or have adverse effects if not taken appropriately.
Regular Eye Exams:
Regular eye exams are crucial for the early detection and prevention of eye conditions, including regenerate. Comprehensive eye exams performed by an eye care professional can help identify any changes in your eye health and detect potential issues before they progress.
During a comprehensive eye exam, your eye care professional will evaluate various aspects of your eye health, including visual acuity, eye pressure, peripheral vision, and the overall health of your eyes. They may also dilate your pupils to get a better view of the internal structures of your eyes, including the lens.
Early detection of any changes in the lens, such as cloudiness or opacity, can help initiate appropriate treatment or preventive measures to slow down the progression of regenerate. Additionally, eye exams can also detect other eye conditions or systemic health issues that may contribute to eye diseases.
The frequency of eye exams may vary depending on your age, overall health, and any specific risk factors. It is generally recommended to have a comprehensive eye exam at least once every two years, or more frequently as advised by your eye care professional. Regular eye exams are an essential component of maintaining good eye health and preventing eye conditions.
What is the Best Treatment for Cataract? :
Cataract surgery, along with the implantation of an intraocular lens, is considered the best and most effective treatment for regenerate. Cataract surgery involves removing the cloudy lens and replacing it with an artificial lens that restores clear vision. The surgery is safe, relatively quick, and has a high success rate in improving vision and quality of life.
By removing the cloudy lens and replacing it with an intraocular lens, cataract surgery can provide a long-term solution for regenerate. The artificial lens is designed to correct vision problems and can address specific refractive errors like nearsightedness, farsightedness, and astigmatism. This allows individuals to regain clear vision and reduces their dependence on glasses or contact lenses.
Cataract surgery is performed on an outpatient basis, meaning you can return home on the same day. The recovery period is usually short, and most individuals experience a significant improvement in their vision within a few weeks. It is important to follow the post-operative care instructions provided by your ophthalmologist and attend follow-up appointments to monitor the healing process and ensure optimal outcomes.
In conclusion, cataract surgery, accompanied by intraocular lens implantation, is the best treatment option for regenerate. It offers a safe and effective solution to restore clear vision and improve overall quality of life.
Surgery:
When conservative measures are no longer effective in managing cataract symptoms or when vision impairment significantly impacts daily activities and quality of life, cataract surgery may be recommended. Cataract surgery is a safe and commonly performed procedure that involves the removal of the cloudy lens and the replacement with an artificial lens known as an intraocular lens (IOL). The surgery is usually performed on an outpatient basis and typically takes only a short amount of time to complete.
During the surgery, a small incision is made in the eye, and specialized tools are used to break up and remove the cloudy lens. Once the cataract is removed, an IOL is inserted into the eye to restore clear vision. The IOL is selected based on individual needs and can correct various vision problems, such as nearsightedness, farsightedness, and astigmatism.
Cataract surgery is generally a safe and effective procedure, with a high success rate in improving vision and quality of life. Most individuals experience a significant improvement in their vision soon after the surgery, although it may take a few weeks for the eyes to fully adjust and for optimal vision to be achieved.
Intraocular Lens (IOL):
During cataract surgery, the cloudy natural lens of the eye is replaced with an artificial lens called an intraocular lens (IOL). Intraocular lenses are designed to restore clear vision and can correct various types of refractive errors, such as nearsightedness, farsightedness, and astigmatism.
There are different types of IOLs available, including monofocal, multifocal, and toric lenses. Monofocal lenses are the most common type and provide clear vision at a single focal point, usually for distance vision. In this case, individuals may still need to wear glasses for near or intermediate tasks. Multifocal lenses, on the other hand, have multiple focal points, allowing for clear vision at different distances, reducing the dependence on glasses. Toric lenses are specifically designed to correct astigmatism.
The choice of IOL depends on various factors, including the individual’s visual needs, lifestyle, and the recommendation of the ophthalmologist. During the preoperative evaluation, the ophthalmologist will discuss the available options and help determine the most suitable IOL for each individual.
Lifestyle Changes:
In addition to cataract surgery, certain lifestyle changes can help improve vision and enhance the overall success of the treatment. Following cataract surgery, it is important to protect the eyes from injury and infection during the recovery period. This can be done by avoiding activities that may put the eyes at risk, such as rubbing the eyes, swimming in pools, or exposing the eyes to dust or other irritants.
Taking proper care of the eyes post-surgery is crucial for a successful recovery. This includes using prescribed eye drops as directed by the ophthalmologist, keeping the eyes clean, and avoiding activities that strain the eyes, such as excessive screen time. It is also important to attend follow-up appointments with the ophthalmologist to monitor the healing process and ensure the best possible outcome.
Additionally, maintaining a healthy lifestyle can support overall eye health and optimize the benefits of cataract surgery. This includes eating a nutritious diet rich in fruits, vegetables, and omega-3 fatty acids, which can provide essential nutrients for eye health. Regular exercise, proper hydration, and adequate sleep also contribute to overall well-being and can positively impact eye health.
Medication:
While cataract surgery is the primary treatment for cataracts, there are currently no medications that can reverse or eliminate cataracts. Medications may be prescribed before or after cataract surgery to manage specific conditions or symptoms associated with cataracts, such as inflammation or elevated intraocular pressure.
Before surgery, your ophthalmologist may prescribe eye drops to reduce inflammation or prevent infection. These medications are typically used in the days leading up to the surgery to prepare the eye for the procedure. Following cataract surgery, antibiotic or anti-inflammatory eye drops may be prescribed to prevent infection and reduce inflammation during the healing process.
It is important to follow the prescribed medication regimen as instructed by your ophthalmologist. If you have any concerns or experience side effects, it is essential to communicate with your healthcare provider.
Natural Remedies:
While there is no scientific evidence to support the effectiveness of natural remedies in reversing or treating cataracts, some people may consider using certain natural supplements or remedies to support overall eye health. It is important to note that these remedies should not replace medical treatment or cataract surgery but can be used as complementary approaches in consultation with your healthcare provider.
Some natural remedies that are commonly discussed in relation to eye health include antioxidant supplements, such as vitamins C and E, beta-carotene, and lutein. These antioxidants are believed to help protect the eyes from oxidative damage. However, it is important to discuss the use of any supplements or natural remedies with your ophthalmologist to ensure their safety and effectiveness, as well as to avoid any potential interactions with medications or adverse effects.
It is crucial to approach natural remedies with caution and rely on evidence-based medical treatments for cataracts, such as cataract surgery. Regular discussions and open communication with your healthcare provider are key to making informed decisions about your eye health.
What are the complications of untreated cataract? :
Untreated cataracts can lead to various complications that can significantly impact an individual’s vision and overall well-being. Some of the potential complications include:
-
Visual Impairment: As cataracts progress, they can cause severe vision loss, making it difficult to perform daily activities and affecting quality of life.
-
Increased Risk of Falls: Cataracts can impair depth perception and reduce clarity of vision, increasing the risk of falls and accidents, especially in older adults.
-
Social Isolation: Vision loss from untreated cataracts can lead to social isolation and decreased participation in activities, leading to a decline in mental and emotional well-being.
-
Depression and Anxiety: The impact of vision loss and reduced independence can contribute to feelings of depression and anxiety in individuals with untreated cataracts.
-
Secondary Eye Conditions: Untreated cataracts can increase the risk of developing secondary eye conditions, such as glaucoma or retinal detachment, which can further compromise vision and require additional treatment.
It is important to prioritize regular eye examinations and seek appropriate treatment, such as cataract surgery, to prevent or minimize the complications associated with untreated cataracts. Early intervention can help preserve vision, enhance quality of life, and reduce the risk of further complications.
Vision Loss:
One of the most significant complications of untreated cataracts is vision loss. As the cataract progresses and the lens becomes increasingly cloudy, it can severely impair vision. Initially, individuals may experience blurred or hazy vision, difficulty reading or performing tasks that require clear vision, and increased sensitivity to glare. As the cataract worsens, vision loss can become more pronounced, impacting daily activities and overall quality of life.
Without appropriate treatment, such as cataract surgery, the vision loss caused by cataracts can continue to deteriorate. It can lead to a significant decline in visual acuity, making it challenging to engage in activities that were once enjoyed. In severe cases, untreated cataracts can cause complete vision loss, greatly affecting independence and overall well-being.
Driving:
Untreated cataracts can have a profound impact on an individual’s ability to drive safely. As cataracts progress, they can cause a variety of vision problems, including blurred vision, decreased contrast sensitivity, and increased sensitivity to glare. These visual impairments can make it difficult to see road signs, judge distances accurately, and react to unexpected situations while driving.
Driving with untreated cataracts poses risks not only to the individual but also to other road users. Impaired vision can lead to poor depth perception, compromised peripheral vision, and difficulty seeing objects clearly, all of which can contribute to accidents or unsafe driving situations.
It is crucial for individuals with cataracts to prioritize their safety and the safety of others by seeking appropriate treatment, such as cataract surgery, as recommended by their healthcare provider. Cataract surgery can significantly improve vision and restore the ability to drive safely, allowing individuals to maintain their independence and mobility.
Secondary Cataracts:
One potential complication that can arise after cataract surgery is the development of secondary cataracts, also known as posterior capsular opacification (PCO). Secondary cataracts occur when the back portion of the lens capsule, which remains intact during cataract surgery, becomes cloudy over time. This can cause vision to become blurred or hazy, similar to the symptoms experienced with primary cataracts.
Secondary cataracts occur in a small percentage of individuals who have undergone cataract surgery. The risk of developing secondary cataracts can vary depending on factors such as age, underlying health conditions, and the type of intraocular lens used during the surgery.
Fortunately, secondary cataracts can be easily treated with a quick and painless outpatient procedure called YAG laser capsulotomy. During this procedure, a laser is used to create a small opening in the cloudy capsule, allowing light to pass through and restoring clear vision. YAG laser capsulotomy is a safe and effective treatment that can provide long-lasting improvement in vision.
It is important for individuals who have undergone cataract surgery to be aware of the possibility of secondary cataracts and to promptly seek evaluation and treatment if they experience any changes in their vision.
Glaucoma:
Although cataracts and glaucoma are two separate eye conditions, they can occur simultaneously, and the presence of cataracts can complicate the management of glaucoma. Glaucoma is a group of eye diseases characterized by damage to the optic nerve, often associated with increased pressure inside the eye. It can lead to gradual vision loss and, if left untreated, can cause permanent blindness.
In some cases, the presence of cataracts can affect the accurate measurement of intraocular pressure, which is an important aspect of glaucoma diagnosis and management. Cataracts can also make it more challenging to visualize the optic nerve and assess the progression of glaucoma.
Additionally, some glaucoma medications, such as corticosteroid eye drops, can contribute to the development or progression of cataracts. Therefore, it is important for individuals with both cataracts and glaucoma to work closely with their ophthalmologist to develop a comprehensive treatment plan that addresses both conditions.
Regular eye examinations and close monitoring of both cataracts and glaucoma are essential to ensure early detection and appropriate management of these conditions. This may involve a combination of cataract surgery and glaucoma treatments, such as eye drops, oral medications, laser procedures, or surgery, depending on the severity and progression of each condition.
Retinal Detachment:
Retinal detachment is a potentially serious complication that can occur in individuals with untreated cataracts. The retina is a thin layer of tissue located at the back of the eye that is responsible for detecting light and sending visual signals to the brain. If the retina becomes detached, it can result in a partial or complete loss of vision in the affected eye.
Cataracts can increase the risk of retinal detachment due to several factors. The presence of a dense cataract can make it difficult for an eye doctor to thoroughly examine the retina and detect any signs of retinal tears or detachment. In addition, the natural aging process and changes in the eye associated with cataracts can contribute to the weakening of the retina and the development of tears or breaks.
If retinal detachment occurs, it is considered a medical emergency, and immediate intervention is required to prevent permanent vision loss. Surgery, such as a vitrectomy or retinal reattachment procedure, is typically performed to reposition and secure the detached retina. Prompt diagnosis and treatment are crucial for achieving the best possible outcome in cases of retinal detachment.
To minimize the risk of retinal detachment and other complications, individuals with cataracts should undergo regular eye examinations and follow the recommendations of their eye care professional. Seeking timely treatment, such as cataract surgery, can help reduce the risk of complications and preserve vision.
Related Links
Conclusion:
In conclusion, the condition known as cataract can have a significant impact on vision and overall quality of life if left untreated. This common eye disorder involves the clouding or opacification of the eye’s lens, resulting in various visual symptoms such as blurred vision, decreased color perception, and increased sensitivity to glare. Fortunately, medical advancements have led to effective treatments, such as surgical intervention and lifestyle modifications, that can help regenerate clear vision and enhance the well-being of individuals affected by cataracts.
Cataract surgery, a widely performed procedure, involves the removal of the cloudy lens and the implantation of an artificial lens to restore visual clarity. The surgical process is generally safe and offers promising outcomes. It is typically performed on an outpatient basis, allowing for a swift recovery and a prompt return to daily activities. By considering cataract surgery, individuals can regenerate their vision, regain independence, and improve their overall quality of life.
Regular eye examinations are vital in the management of cataracts. Early detection of the condition allows for timely intervention and appropriate treatment planning. Monitoring the progression of cataracts through routine check-ups enables healthcare professionals to recommend the most suitable time for surgery. It is essential to address any concerns or symptoms promptly to prevent complications and achieve the best possible visual regeneration.
Q: 1. Can cataracts be prevented?
A: While complete prevention of cataracts is not possible, certain lifestyle choices and habits can potentially delay their onset or slow down their progression. Maintaining a healthy lifestyle, protecting the eyes from harmful UV radiation, and avoiding smoking are factors that may contribute to reducing the risk of developing cataracts.
Q: 2. Are there alternatives to surgery for treating cataracts?
A: Currently, cataract surgery is the most effective treatment for advanced cataracts. However, in the early stages, visual symptoms can often be managed with prescription eyeglasses or contact lenses, which may help improve vision temporarily.
Q: 3. How long does cataract surgery take?
A: The duration of cataract surgery varies, but the procedure typically lasts between 15 and 30 minutes per eye. It is performed under local anesthesia, and most individuals can return home on the same day.
Q: 4. What is the recovery period after cataract surgery?
A: Recovery following cataract surgery is generally rapid. Many individuals experience improved vision within a few days, with full recovery achieved within a few weeks. During the recovery period, it is crucial to follow the post-operative instructions provided by the healthcare professional.
Q: 5. Can cataracts recur after surgery?
A: Once a cataract is surgically removed and replaced with an artificial lens, it does not regenerate. However, in some cases, a condition known as posterior capsular opacification (PCO) may develop, leading to a gradual clouding of the lens capsule. Fortunately, PCO can be easily treated with a simple and painless laser procedure.
More Links
|
Once a cataract is surgically removed and replaced with an artificial lens, it does not regenerate. |