Leprosy: The Latest Breakthroughs (2024) – Unforgettable Insights into Causes, Symptoms, and Treatment

Overview of Leprosy.
Leprosy, also known as Hansen’s disease, is a chronic infectious disease caused by the Mycobacterium leprae bacteria. This ancient affliction primarily affects the skin and peripheral nerves, leading to a spectrum of symptoms ranging from mild skin lesions to severe nerve damage and deformities if left untreated. Historically, leprosy has carried a heavy social stigma, resulting in discrimination and isolation for those affected. However, with advancements in medical science and increased awareness, efforts to combat leprosy have made significant progress in recent years, offering hope for improved diagnosis, treatment, and ultimately, the eradication of this debilitating disease.
Despite significant strides in understanding and managing leprosy, challenges persist, particularly in regions with limited access to healthcare and resources. Stigma and misconceptions surrounding the disease continue to hinder early detection and treatment, prolonging the suffering of those affected. However, ongoing global efforts, spearheaded by organizations like the World Health Organization (WHO), focus on early diagnosis, multidrug therapy, and community-based interventions to reduce transmission and mitigate the impact of leprosy. By fostering collaboration, raising awareness, and advocating for the rights of individuals affected by leprosy, we can work towards a future where this ancient scourge no longer poses a threat to public health and well-being.
What are the main causes of leprosy?
The primary cause of leprosy is the Mycobacterium leprae bacteria, which primarily targets the skin and nerves. It is transmitted through respiratory droplets from an infected person, although the exact mechanisms of transmission are not fully understood. Let’s delve into the causes of leprosy and explore the transmission methods in more detail:
Mycobacterium leprae Bacteria:
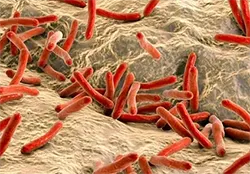
Mycobacterium leprae, also known as the leprosy bacillus or Hansen’s bacillus, stands as the primary culprit behind leprosy. This bacterium is characterized by its acid-fast, Gram-positive, rod-shaped structure and targets various parts of the body, including the skin, eyes, nose, muscles, and peripheral nerves. Unlike its relative, Mycobacterium tuberculosis, Mycobacterium leprae cannot be grown in cell-free laboratory media due to gene deletion and decay, relying heavily on its host for nutrients. Interestingly, natural hosts for this bacterium include humans, nine-banded armadillos, and red squirrels. Within the host, it primarily infects macrophages and Schwann cells, often forming a palisade within lesions.
Transmission Methods: The exact route of transmission of leprosy is not fully understood, but it is believed to spread primarily through respiratory droplets expelled from the coughing or sneezing of an infected person. Other risk factors for developing leprosy include close contact with an infected individual, reduced immune function, malnutrition, and living in poverty. It’s important to note that leprosy is not highly contagious, and casual contact such as shaking hands does not readily spread the disease. Within the host, the bacteria primarily infect macrophages and Schwann cells.
Remember, early diagnosis and treatment are crucial for preventing complications and promoting social inclusion. Leprosy is curable with multidrug therapy that includes antibiotics like dapsone, rifampicin, and clofazimine.
What are the 3 main symptoms of leprosy?
Leprosy presents with a wide range of symptoms, ranging from mild skin lesions to severe nerve damage. Early signs may include discolored patches of skin and numbness in affected areas. As the disease progresses, patients may experience deformities and loss of sensation in their extremities. Let’s explore the symptoms associated with leprosy in more details:
1. Skin Lesions and Disfigurement:
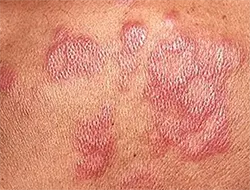
Skin manifestations of the condition often include discolored patches, which may present as red areas or exhibit a loss of pigmentation. These patches, typically flat in appearance, may also lack sensation. Additionally, individuals affected by the condition may develop growths or nodules on their skin, varying in size and affecting nerves, skin, and organs. The skin can also undergo changes in texture and appearance, becoming thick, stiff, or dry. Painless ulcers may form on the soles of the feet, often unnoticed due to reduced sensation, and painless swelling or lumps may develop on the face or earlobes, potentially leading to disfigurement.
2. Nerve Damage and Loss of Sensation:
Nerve damage is a hallmark of the condition, leading to various neurological symptoms. Affected individuals may experience numbness in specific areas of the skin due to nerve damage. Muscle weakness or paralysis, particularly in the hands and feet, may occur as a result of nerve impairment. Enlarged nerves are a common feature, particularly around the elbow, knee, and sides of the neck. Furthermore, facial nerves can be affected, potentially resulting in eye problems and, in severe cases, blindness.
3. Other Complications:
In addition to skin and nerve-related symptoms, individuals with the condition may experience other complications. Thick or stiff skin may develop as a consequence of nerve damage, leading to further impairment. Loss of eyebrows or eyelashes may occur, resulting in aesthetic changes. Nasal congestion and nosebleeds may also manifest due to mucous membrane involvement. In advanced cases, individuals may experience paralysis and crippling of the hands and feet, shortening of toes and fingers due to reabsorption, blindness, disfigurement of the nose, and permanent damage to the hands and feet.
Remember, early diagnosis and treatment are crucial to prevent complications and promote better outcomes. If you suspect any symptoms related to leprosy, seek medical attention promptly.
What is the diagnostic tool for leprosy?
Diagnosing leprosy typically involves a combination of clinical examination and laboratory tests. Healthcare professionals may conduct skin biopsies or nerve function tests to confirm the presence of the bacteria. Let’s delve into the diagnosis of the condition and the tools utilized for it in more detail:
Clinical Examination:
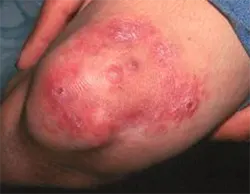
Clinical diagnosis plays a pivotal role in identifying the condition, particularly in regions with limited access to laboratory facilities. Healthcare professionals rely on specific signs during examination, including the definite loss of sensation observed in pale (hypopigmented) or reddish skin patches. Additionally, thickened or enlarged peripheral nerves, often accompanied by loss of sensation and muscle weakness, serve as key indicators. Microscopic detection of bacilli in a slit-skin smear is another essential aspect of clinical examination. The WHO expert committee defines a case of the condition based on these cardinal signs, facilitating accurate diagnosis even in resource-constrained settings.
Laboratory Tests:
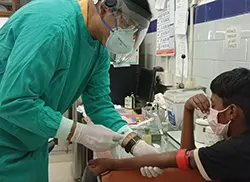
Laboratory tests complement clinical examination and provide additional confirmation of the diagnosis. The slit-skin smear (SSS) procedure involves obtaining a sample of affected skin and testing it for the presence of acid-fast bacilli using stains like Ziel-Neelsen or Fite stain. This method is particularly useful for diagnosing multibacillary cases of the condition. Histopathology, involving skin or nerve biopsy from the edges of active patches, demonstrates the presence of bacilli and aids in confirming the diagnosis. While PCR (Polymerase Chain Reaction) is currently not as reliable, it may be used in specific cases to further support the diagnosis.
What are the types of leprosy?
Indeterminate Leprosy
Indeterminate Leprosy represents the mildest manifestation of the disease. Let’s explore its characteristics in detail:
-
Skin Lesions: Individuals diagnosed with indeterminate leprosy typically exhibit one or a few skin lesions. These lesions may vary in appearance but often present as hypopigmented or reddish patches on the skin. Unlike more severe forms of the disease, the skin lesions in indeterminate leprosy are limited in number and usually have well-defined borders.
-
Nerve Involvement: One notable characteristic of indeterminate leprosy is the absence of definite nerve involvement. Unlike other types of leprosy, where nerve damage is more pronounced and can lead to sensory loss or muscle weakness, indeterminate leprosy typically spares the nerves. This distinguishes it as a milder form of the disease with fewer neurological complications.
-
Spontaneous Resolution: Interestingly, indeterminate leprosy often resolves spontaneously without the need for specific medical treatment. In some cases, the skin lesions may fade over time, and individuals may experience complete recovery without experiencing further progression of the disease. This aspect highlights the relatively benign nature of indeterminate leprosy compared to more advanced forms.
In summary, indeterminate leprosy is characterized by minimal skin involvement and lacks the pronounced nerve damage seen in other forms of the disease. Early detection and monitoring are essential to ensure timely intervention if needed.
Tuberculoid Leprosy
Tuberculoid Leprosy stands as one of the two major forms of the condition. Let’s delve into its details:
-
Definition: Tuberculoid leprosy is a distinct form of the disease characterized by solitary skin lesions that are asymmetrically distributed. These lesions are typically few in number and display well-demarcated edges. Despite the presence of skin lesions, early and marked nerve damage may occur in individuals with this form of leprosy. Notably, tuberculoid leprosy tends to heal spontaneously without the need for specific medical intervention.
-
Clinical Features:
- Skin Lesions: Skin lesions associated with tuberculoid leprosy present as well-defined, hypo-pigmented patches or plaques on the skin. These lesions may exhibit numbness due to nerve involvement, and their edges are clear and sharply demarcated.
- Nerve Involvement: Unlike other forms of leprosy, nerve damage is minimal or absent in tuberculoid leprosy. There is no pronounced nerve thickening observed, distinguishing it from more severe forms of the disease.
- Immune Response: Tuberculoid leprosy is characterized by a strong immune response against the causative bacteria, Mycobacterium leprae. The immune system attempts to contain the infection, resulting in the distinctive clinical features associated with this form of leprosy.
-
Prognosis: Tuberculoid leprosy generally carries a better prognosis compared to other forms of the disease. With early diagnosis and appropriate treatment, patients can experience improvement in their condition, and in some cases, spontaneous healing of skin lesions may occur.
Remember, early detection and timely intervention are crucial for better outcomes in individuals with tuberculoid leprosy.
Borderline Tuberculoid Leprosy
Borderline Tuberculoid Leprosy represents an intermediate form of the disease, lying between tuberculoid and borderline lepromatous leprosy. Let’s delve into its details:
-
Definition: Borderline tuberculoid leprosy represents an intermediate stage between two primary forms of the condition. It shares characteristics of both tuberculoid and lepromatous leprosy but occupies a distinct clinical entity.
-
Clinical Features:
- Skin Lesions: Borderline tuberculoid leprosy is marked by the presence of multiple skin lesions. These lesions, resembling those observed in tuberculoid leprosy, are more numerous and can appear anywhere on the body. They often display hypo-pigmentation and may have irregular borders.
- Sensation: Some skin lesions associated with borderline tuberculoid leprosy may exhibit partial loss of sensation due to nerve involvement. However, sensory impairment in this form of the disease is typically less severe compared to advanced stages.
- Nerve Involvement: While nerve involvement is more pronounced than in tuberculoid leprosy, it remains less severe than in other forms. Nerve damage can lead to sensory deficits and motor impairment but to a lesser extent.
-
Immune Response: Borderline tuberculoid leprosy is characterized by a compromised cell-mediated immune response to Mycobacterium leprae. This results in widespread bacterial infiltration of the skin, nerves, and other tissues, contributing to the clinical manifestations observed.
Remember, early diagnosis and appropriate treatment are crucial for better outcomes in individuals with this condition. Multidrug therapy, including antibiotics such as dapsone, rifampicin, and clofazimine, remains the standard treatment protocol.
Borderline Lepromatous Leprosy
Borderline lepromatous leprosy serves as an intermediate form bridging tuberculoid and lepromatous leprosy, sharing clinical features of both. This subtype is characterized by numerous skin lesions, variable in appearance and distribution across the body, resembling those of lepromatous leprosy but exhibiting greater variability. Sensory loss can vary in severity due to nerve involvement, while nerve damage, although more extensive than in tuberculoid leprosy, is less severe than in pure lepromatous leprosy cases. Individuals with borderline leprosy often display intermediate immune responses to Mycobacterium leprae, with widespread bacterial infiltration of skin, nerves, and organs. Early diagnosis and appropriate treatment, including multidrug therapy comprising antibiotics like dapsone, rifampicin, and clofazimine, are essential for optimal outcomes.
Lepromatous Leprosy
Lepromatous leprosy, one of the two primary forms of the disease alongside tuberculoid leprosy, represents the most severe end of the leprosy spectrum. Clinical manifestations include widespread skin lesions appearing as numerous nodules, plaques, or thickened areas, often accompanied by a spongy texture due to bacterial infiltration. Extensive involvement of peripheral nerves leads to sensory loss, muscle weakness, deformities, and neuropathy. Weak immune responses against Mycobacterium leprae result in uncontrolled bacterial dissemination throughout the body, attacking internal organs, bones, joints, and marrow. Physical degeneration can lead to the disappearance of eyebrows, the emergence of spongy tumor-like swellings, loss of feeling in fingers and toes, amputation, and blindness, among other complications.
Treatment for lepromatous leprosy typically involves a regimen of antibiotics such as dapsone, rifampicin, and clofazimine for a duration of 2–5 years. Early detection is crucial to prevent irreversible physical and neurological damage, even though both forms of leprosy are curable. Family members, particularly children, are at the highest risk of infection, emphasizing the importance of prompt medical attention and intervention if symptoms suggestive of leprosy arise. Early diagnosis and timely treatment are paramount for improving outcomes and preventing severe complications associated with lepromatous leprosy.
What are Treatment Options for Leprosy
Multidrug therapy (MDT) serves as the primary treatment for Hansen’s Disease. It combines various antibiotics, including dapsone, rifampicin, and clofazimine (added for some types of the disease). Treatment duration varies depending on the type of the condition. For the paucibacillary form, which involves a low bacterial load, dapsone and rifampicin are administered concurrently. In contrast, for the multibacillary form, which involves a higher bacterial load, clofazimine is added to rifampicin and dapsone. The treatment typically spans one to two years, and completing the prescribed regimen is imperative for achieving a cure.
Surgery plays a vital role in managing complications stemming from Hansen’s Disease. While it doesn’t directly address the disease itself, surgical interventions are essential for addressing associated complications. Neural surgery becomes necessary for patients experiencing persistent nerve pain, while reconstructive surgery helps correct deformities induced by the disease. These surgical procedures not only improve physical functionality but also enhance cosmetic appearance, enabling individuals to reintegrate into society and combat stigma. Remember, early diagnosis, timely intervention, and strict adherence to treatment protocols significantly contribute to favorable treatment outcomes.
Recent Breakthroughs in Leprosy Research
Recent breakthroughs in Hansen’s Disease research, particularly in genomic studies, have illuminated significant aspects of the disease’s pathogenesis. Genome-wide association studies (GWAS) have played a pivotal role in identifying numerous susceptibility genes linked to Hansen’s Disease. Many of these genes are intricately involved in immune responses, shedding light on the immunogenetic underpinnings of the condition. This deeper understanding of the genetic factors influencing host immune reactions to Mycobacterium leprae is crucial for advancing our management and control strategies against Hansen’s Disease. By deciphering the genetic mechanisms at play, researchers can potentially uncover novel therapeutic targets and personalized treatment approaches tailored to individual genetic profiles.
Moreover, advancements in immunotherapy offer promising avenues for enhancing the immune response against Hansen’s Disease. Researchers are exploring various immunotherapeutic strategies aimed at bolstering the body’s defenses against the pathogen. Among these approaches, investigations into the use of corticosteroid injections for treating leprosy-associated neuritis have shown promise. Additionally, cyclophosphamide pulse therapy is being studied as a potential treatment for managing chronic and refractory cases of erythema nodosum leprosum, a debilitating type of leprosy reaction. These developments represent significant strides in the quest for more effective treatments for Hansen’s Disease, offering hope for improved outcomes and quality of life for affected individuals.
Conclusion:
In conclusion, the recent advancements in research related to Hansen’s Disease, particularly in genomic studies and immunotherapy developments, hold tremendous promise for the future of disease management. By unraveling the genetic intricacies underlying host immune responses and identifying novel susceptibility genes, researchers are paving the way for more targeted and personalized treatment approaches. Additionally, the exploration of immunotherapeutic strategies, such as corticosteroid injections and cyclophosphamide pulse therapy, offers hope for improved outcomes and enhanced quality of life for individuals affected by the condition. These breakthroughs signify a significant step forward in our understanding and combat against Hansen’s Disease, underscoring the importance of continued research efforts in the pursuit of better treatments and ultimately, eradication of the disease.
FAQs:
Q: What is Hansen’s disease?
Answer: Hansen’s disease, commonly known as leprosy, is a chronic infectious disease caused by the bacterium Mycobacterium leprae. It primarily affects the skin and peripheral nerves, leading to skin lesions and nerve damage.
Q: How is Hansen’s disease transmitted?
Hansen’s disease is believed to spread through respiratory droplets when an infected person coughs or sneezes. However, it’s not highly contagious, and the majority of people exposed to the bacteria do not develop the disease. Close and prolonged contact with an untreated individual with Hansen’s disease is typically necessary for transmission.
Q: What are the symptoms of Hansen’s disease?
Answer: Symptoms of Hansen’s disease vary depending on the type and severity of the infection. Common signs include skin lesions, numbness or loss of sensation, muscle weakness, and nerve thickening. In advanced cases, deformities may occur, such as clawed hands or foot drop. Additionally, individuals may experience eye problems and nasal congestion.
Q: Is Hansen’s disease curable?
Answer: Yes, Hansen’s disease is curable with multidrug therapy (MDT), which involves a combination of antibiotics such as dapsone, rifampicin, and clofazimine. The duration of treatment varies based on the type of Hansen’s disease and its severity. Early diagnosis and prompt initiation of treatment are crucial to prevent complications and achieve a cure.
Q: How can Hansen’s disease be prevented?
Answer: Preventive measures for Hansen’s disease primarily focus on early detection and treatment of cases, as well as providing information and education to communities. Additionally, the Bacillus Calmette-Guérin (BCG) vaccine has shown some protective effect against Hansen’s disease in areas where it is endemic. Public health efforts also include contact tracing and screening of household contacts of individuals diagnosed with Hansen’s disease to identify and treat new cases promptly.